31 Jul Microdiscectomy and Low Back Pain: Failed Back Surgery Syndrome
Sometimes a microdiscectomy is necessary, but what happens when it fails?
Pretend with me for a moment that you are experiencing severe low back pain, so bad that your general physician sends you for an MRI to check out what is going on.
They come back and tell you that you need a microdiscectomy because your back is all messed up.
What do you do?
Do you get a microdiscectomy?
Here, we will look into what happens when back surgery fails.
A Diagnosis of Failed Back Surgery Syndrome (FBSS)
A microdiscectomy that does NOT make your pain go away is called Failed Back Surgery Syndrome (FBSS) by The World Health Organization.
This condition is regarded as a major healthcare problem that should be considered a public health crisis according to researchers.
It’s so prolific that the diagnostic coding system doctors use to communicate with health insurance companies, The International Statistical Classification of Diseases and Related Health Problems (aka ICD-10), has a billable specific code for this syndrome.
M96.1.
The code allows your medical providers to be reimbursed for your care after your microdiscectomy fails.
Researchers generally consider FBSS as a syndrome in which patients are affected by either new, recurrent, or persistent pains in the low back after microdiscectomy.
According to the medical literature:
Up to HALF of all patients who undergo low back surgery don’t get better, and many get worse.
Why?
What are the most common causes of FBSS?
What Causes a Microdiscectomy to Fail?
Research shows that there are multiple causes to FBSS, and the most common include pre-operative, operative and post-operative factors.
Preoperative factors include things like:
- psychological factors – are you overly stressed about your pain?
- social factors – are you getting surgery because your husband or wife insists that you do?
- poor surgeon selection
- poor surgical planning
- whether the surgery planned is a revision surgery of a previously diagnosed FBSS case
Operative factors includes:
- poor decompression – did the surgery fulfill it’s purpose?
- instability related to an aggressive surgical approach
- even an INCORRECT level of the spine being operated on!
Post-operative factors includes:
- recurrent disc herniation
- diseases of other spinal segments
- balance issues
- curvature issues
- excessive scarring to the nerve roots
- …and ADHESION causing nerve root entrapment.
Wait! Adhesion!?
What is adhesion?
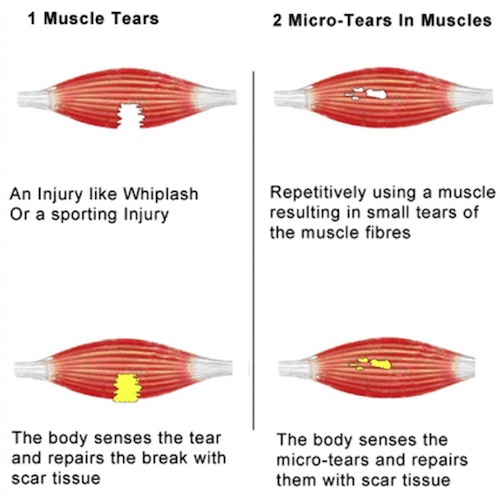
Adhesion is like glue which forms in response to injury or damage to the body’s tissues. When healthy tissue has a build up of this glue-like stuff, it’s not longer able to function properly.
Depending on where adhesion forms, nerves can become entrapped as well.
It’s no wonder that the top two treatments to combat FBSS are adhesionolysis and nerve pain medications like gabapentin, but we will get back to that later!
So what if back surgery fails?
What are the consequences? Why does it matter?
Opioids and The Dangers of the Wrong Treatment
There are grave consequences of getting the wrong treatment that leads to worsening pain and potentially even opioids.
This is why it is SO IMPORTANT to avoid surgery if possible by getting the correct diagnosis ASAP.
Some of the more severe consequences of microdiscectomy gone wrong are:
- disability
- chronic pain
- addiction leading to overdose and death
Lets just go back to playing pretend for a moment and imagine that now you have had your microdiscectomy, you are in worse pain than ever and no amount of medication you are being prescribed is helping you.
You take the medication anyway because you are desperate.
You have missed significant amounts of time at your job, and are now at risk of being jobless.
Not only are there health related consequences, but there are some significant economic consequences to consider like increased insurance premiums, missed work and productivity, and economic hardship.
These factors are estimated to cost the economy over a BILLION dollars annually!
One of the more significant health related consequences to FBSS is chronic pain.
Up to 62% of patients with FBSS use opioids for their pain even though the research demonstrates that the most common cause of pain after FBSS is nerve generated, which opioids have little to no effect on.
It is important to understand the consequence of taking opioids for FBSS.
Opioids will cross the blood brain barrier once in our system, causing them to have a very strong effect of reward on the neurochemistry of the brain which research has proven causes tolerance and addiction.
More than 20% of pain patients with an opioid addiction are FBSS patients!
That’s just addiction.
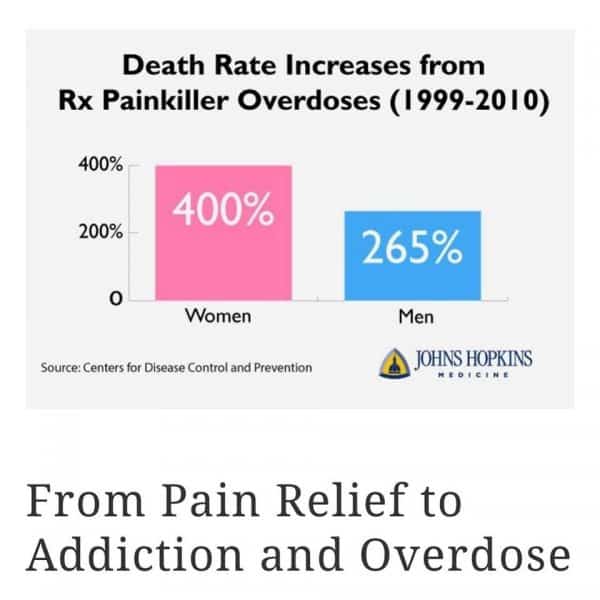
Death from overdose has becoming a worsening issue over the past two decades according to Johns Hopkins University.
Despite there being no clear indication and a lack of demonstrable efficacy for spinal fusion, in a 10 year time period there was a 220% increase in spinal fusion surgeries.
International research data shows that the rate of back surgery in the USA is at least 40% higher than any other country. Compared to some countries, even 4-5x higher!
Incredibly enough, the research has also shown us that when compared to other conditions which cause chronic pain like rheumatoid arthritis, FBSS patients experience:
- greater levels of pain,
- lower quality of life,
- higher levels of disability and
- higher rates of unemployment.
One high quality research study confirmed that FBSS patients experience poorer levels of health related quality of life compared with other chronic diseases such as CHF, and even worse than those with long term Type 2 diabetes!
Going back to the what if this was you scenario, would you want to be addicted to opioids? Or would you want a better way to get out of pain?
Adhesion Is the Missing Block to Your Pain Relief
Several studies determined that the only treatment for FBSS with an A grade, meaning it demonstrated the greatest amount of pain relief, and functional improvements in FBSS overall – was “adhesionolysis”, THE REMOVAL OF ADHESION!
This is what the removal of adhesion looks like with Manual Adhesion Release (TM) to the low back muscles.
Or Manual Adhesion Release (TM) to the psoas muscles on the front of your spine.
Other treatment methods like epidural blocks had a recommendation grade of C, and repeat surgery a grade of D, and other treatments like steroids, NSAIDS and opioids were so bad they didn’t even get a grade, yet these treatments are prescribed routinely to treat FBSS, far more commonly than adhesion removal is!
Failed back surgery syndrome from a microdiscectomy that didn’t work is fast becoming an epidemic in modern medicine with many causes, and serious consequences not only for your health, but for the greater economy as a whole.
Sometimes microdiscectomy is necessary, and its extremely important to consult with highly qualified surgeons when this is the case.
Adhesion plays a significant role not only in chronic back pain, but especially in patients with FBSS. If it were you, knowing what you know now, would you want your adhesion removed? Or would you want to stay on the chronic pain merry-go-round?
Ready to find a Manual Adhesion Release Specialist? Find one on Integrative Diagnosis’s Find a Provider Feature.
👉Do you live in the tri-state area of NJ, NYC, PA? Barefoot Rehab is the ONLY clinic certified to find and fix adhesion within 250 miles.
 Have you had a microdiscectomy that didn’t make your pain any better? Tell us about it below.
Have you had a microdiscectomy that didn’t make your pain any better? Tell us about it below.
Research References:
Cho, et. al. Treatment Outcomes for Patients with Failed Back Surgery. Pain Physician 2017; 20:E29-E43
Yaun-Chaun Chen et. al. Narcotic Addiction in Failed Back Surgery Syndrome. Cell Transplantation 2019, Vol. 28(3) 239-247
Rigoard et. al. Optimizing the Management and Outcomes of Failed Back Surgery Syndrome: A Consensus Statement on Definition and Outlines for Patient Assessment. Pain Research and Management. 2019, Article ID 3126464
Sebaaly, et. al. Etiology, Evaluation, and Treatment of Failed Back Surgery Syndrome. Asian Spine Journal 2018; 12(3):574-588
Taylor et. al. The Economic impact of failed back surgery syndrome. Britsh Journal of Pain 2012, 6(4) 174-181


Anthony Fox
Posted at 13:07h, 25 August7 years in of relentless pain I’m starting to lose my mind, had a microdiscectomy to relieve pressure on the nerve after a fall down some stairs whilst working for a removal company, the surgery managed to relieve some of the sciatic pain I was receiving but this pain still persists even after all this time. I take dihydrocodiene at 4 hr intervals to take the edge off but it doesn’t take the pain away for any decent amount of time. Massage to the affected area works well to relieve the discomfort for a short while. My only advice to people who are suffering the same pain is grit your teeth, hold on tight its going to be a rough and long ride. I know pain well I used to bareknuckle fight when I was a younger man but I would swap this pain with that in a heartbeat.
Ben Paladino
Posted at 07:46h, 11 MarchFulltime first Responder with a recent microdiscectomy on my L2/L3 following a slip and fall at work. Prior to surgery my radicular pain was bilateral and severely debilitating. After my MRI and I was told that I had a large disk extrusion was compressing the spinal cord itself rather than a peripheral nerve which was resulting in my unsual bilateral pain. Following surgery the radicular pain on the right side was 100% cured however the left sided pain remains.i wouldn’t wish this on my worst enemy! If anyone has suggestions I would love to hear them.
Dr. Chris
Posted at 23:24h, 12 MarchSorry to hear this Ben. Since you already had surgery, there’s really nothing else to do besides get the adhesions removed.
Here’s a study I found about adhesions around nerve roots this morning.
https://www.nature.com/articles/3101157