20 Sep Frustrated? Piriformis Syndrome Treatment That Works When Your Pain Has Lasted Longer Than 6 Months
If you’re not annoyed and frustrated by the pain in your ass, literally and figuratively speaking, feel free to click through to another piriformis syndrome treatment page.
What I write here is for people who have had butt pain more than 6 months, even though they’ve seen 3-5 other doctors or therapists…
… and tried stretching, strengthening, physical therapy, chiropractic adjustments, ice, heat, electronic stimulation, cortisone shots, steroids, and any other magical cure promised to you.
Still here?
Good.
Between 1-4 out of 10 people will have “sciatica” at least once in their lifetimes. (Source)
The longer you’ve had piriformis syndrome, the harder it is going to be to get your problem fixed (and the more you need to understand why you haven’t been fixed yet).
As with any health condition, it becomes really important that you use your mind to think through the “stories” different doctors tell you when it comes to getting rid of your pain.
Check in with your intuition:
Does what this doctor says is my problem make sense?
Does this doctor seem like an honest person?
If you answered “no” to any of the above, find a doctor who you can answer “yes” to. Until then, you risk spending serious amounts of time, money, and energy trying to get fixed when your intuition knew the answer all along.
Here’s the sarcastic, but very real, Piriformis Syndrome Treatment That Worked story.
What causes Piriformis Syndrome?
Once your pain is severe and you’re completely and utterly annoyed, frustrated, and pissed off by the lack of relief you’ve found in self-treatments and doctor or therapist-driven treatments, I’ve found that most people don’t care what the cause of their Piriformis Syndrome is.
These patients just want the pain gone!
Before I start treating a patient at Barefoot Rehab, it’s super important to be on the same page about the cause of Piriformis Syndrome.
If you don’t understand the cause, then your mind will wander off the path of getting fixed to other possible treatments that provide very temporary relief, potentially making the cause of your Piriformis Syndrome bigger.
First thing you need to know is that any diagnosis with the word “syndrome” in it tells us nothing as far as what the tissue-specific (is it a muscle or bone or cartilage or ligament? etc.) cause of the problem is and therefore, what treatment you should be looking for.
So, what is Piriformis Syndrome actually? Or what surgeons are starting to cut open with their scalpel and call Deep Gluteal Syndrome?
Below is an actual surgery for Sciatic Nerve Decompression for Deep Gluteal Syndrome:
It’s glue sticking your piriformis (or one of the other hip external rotators) to the sciatic nerve.
That glue is known as adhesion in the medical world. The illustration shows the “black stuff” in the muscle on the right as glue within your muscles.
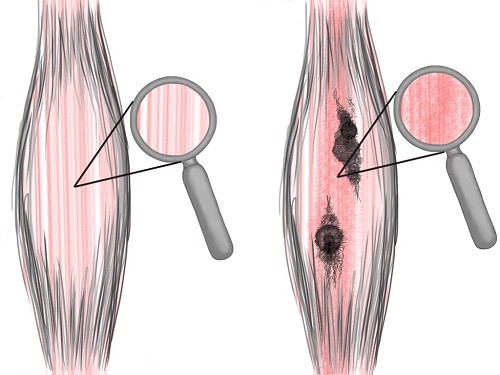
This adhesion forms between your sciatic nerve and one of the hip external rotators:
- piriformis (actually, very uncommon to get adhesion here)
- superior gemellus (most common location to get adhesion)
- inferior gemellus
- obturator externus
- quadratus femoris
Here is Dr. Brady of Integrative Diagnosis explaining how nerves get stuck to muscles. Keep reading and I’ll show you an actual treatment for Piriformis Syndrome with BEFORE and AFTER ranges of motion.
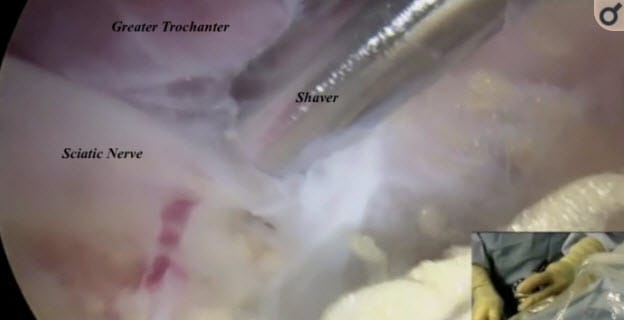
In the image below (source), the gluteus maximum has been taken off the image. The sciatic nerve is the thick black line. In your body, it’s as thick as your index finger. It’s quite easy for an expert doctor to feel if the nerve moves or if it’s glued down by what feels like a wad of gum called adhesion.
Orthopedic surgeons have confirmed that adhesion (or what they call “fibrous bands”) on the right side (or lateral side) of the nerve is MOST COMMON.
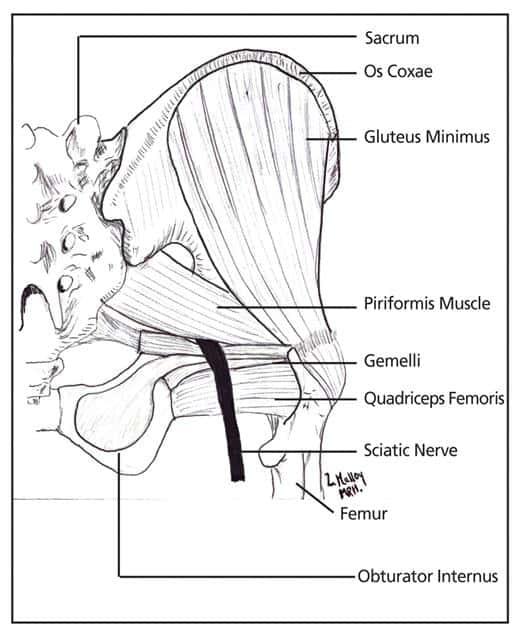
Photo courtesy of http://jaoa.org/article.aspx?articleid=2093614
Anyone who is reading this and who has had “piriformis syndrome” for less than 6 months with mild pain and the pain was helped by the standard advice of:
- ice
- heat
- stretching
- physical therapy
- electronic stimulation
- massage therapy
- medication …
… either never had adhesion in this location or had a small amount of it that hasn’t gotten thick enough to cause more intense pain.
Stretching and movement can get rid of tiny bits of adhesion.
There are only two ways to get rid of thicker wads of adhesion.
More on that below.
Now that we understand adhesion, we have to see if you actually have adhesion by determining if Piriformis Syndrome is your correct diagnosis.
How do you know if “Piriformis Syndrome” is the Correct Diagnosis?
Getting the correct diagnosis for your pain, especially when it’s lasted more than 6 months, is a difficult thing to accomplish.
The wrong diagnosis can leave you feeling silly, wondering how you ever got into such a predicament.

The human body is quite the puzzle and it’s not easy for doctors with regular orthopedic, chiropractic, medical, or physical therapy educations to get hard answers right.
Educational institution’s job is to graduate doctors, not create experts.
A discussion of what piriformis syndrome “looks like” is necessary.
If it looks like a duck and quacks like a duck, is it a duck?
It’s a good thing that chimeras (those magical animals that are actually 3 MULTIPLE ANIMALS in ONE) don’t actually exist.
Real-life lion-goat-snakes would scare the bejeesus out of most of us.
Unfortunately, chimeras do exist when it comes to pain, as much as you might not want to believe it.

Your chimera might be the possibility that you have MULTIPLE problems going on, which will confound the case. If it sounds like you do, I highly recommend you find a musculoskeletal specialist to manage your case for you.
With that said, let’s dive in to getting your diagnosis right.
Let’s assume your Piriformis Syndrome is just a normal duck.
Piriformis Syndrome will typically look like this:
Location of pain (can be any combination of the below locations:
- Your butt check (you’d rate it at least a “5” on the 0-10 pain scale, where “0” is no pain and “10” is the worst pain ever)
- Right down the back of the middle of your thigh
- Right down the back of the middle of your calf OR down the outside of your calf (not the inside)
- Along the top or bottom of your boot.
Location of nerve symptoms: Possible numbness or tingling in your butt cheek or down the back of your thigh, usually not past the knee.
What makes the pain worse?
- Walking for a period of time
- Stretching your “hamstring” like touching your toes or doing a hamstring stretch lying on your back.
- Lying in bed at night
- Sitting for a period of time (i.e. caused by direct pressure to the location of adhesion), especially directly on the painful side
Notice in the image below, the individuals are leaning on the opposite hip.
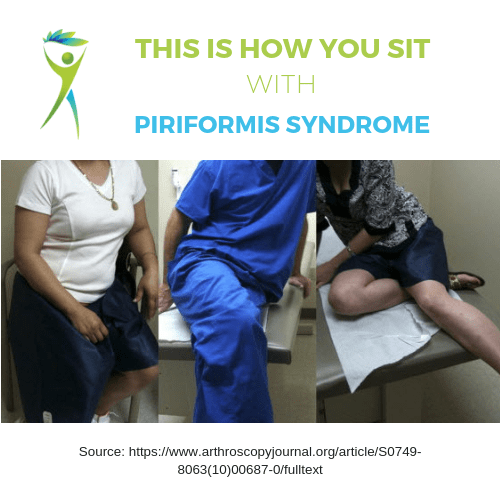
Can you test yourself at home?
- Yes, with the Hamstring Stretch Test
Get your friend, lie on your back, have them straighten your knee and bring your hamstring as high as you can go until you feel not a mild, but at least a “moderate” intensity stretch or pain symptom.
A great confirmation that you have Piriformis Syndrome is when this test reproduces pain precisely in your butt.
“Good” range is higher than 45 degrees (above a 50% grade).
“Bad” range is lower than 45 degrees (below a 50% grade).
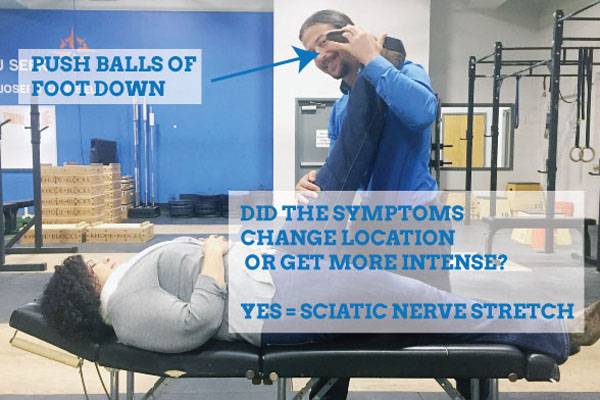
At your end range, have your friend push down on the ball of your foot 1-2″ (no more than this).
If the pulling or pain INCREASES, you can be sure that your sciatic nerve is the problem. We don’t yet know if the sciatic nerve is being pulled at your piriformis, hamstring, or low back. Your expert adhesion doctor will confirm that for you.
If the symptoms INCREASED right in your butt, the diagnosis of Piriformis Syndrome becomes more probable.
Are there any other tests you can do?
- Ultrasound of the sciatic nerve can determine if your sciatic nerve is swollen (Kara et al.)
Piriformis Syndrome will NOT look like this:
Any of the below data points that are true either:
- Lessens the probability that you have Piriformis Syndrome … or …
- Introduces the possibility that you have a chimera (MULTIPLE problems instead of just ONE problem)
Location of pain:
- Your low back
- Down the inside, front, or outside of your thigh
- Down the inside of your calf (not the outside)
Location of nerve symptoms: Numbness or tingling in the front of your thigh, shin, or foot.
What makes the pain worse?
- Standing
- Movements of the spine
Can you test yourself at home?
- Yes, with the Pencil Test and the Touch Your Toes Test
The Pencil Test is like a blood pressure test for your low back. It tells you how healthy or unhealthy your low back is, just like blood pressure tells you how much risk you have for a heart attack or not.
In Barefoot Rehab, we use a pencil ruler to get an exact measurement.
You can just take a simple pencil and grade 1 observation?
- Is the pencil flat against your low back with a grade of 90% through 65% below (the higher the grade, the healthier your low back is)?
- The better your grade is, the MORE likely you have Piriformis Syndrome.
- Or is there space under the pencil with a grade of 40% (the lower the grade, the more likely you have a disc problem).
- The worse your grade is, the LESS likely you have Piriformis Syndrome.
A very healthy low back – 90% function (fxn) – Notice the pencil is flat for 1.5″:
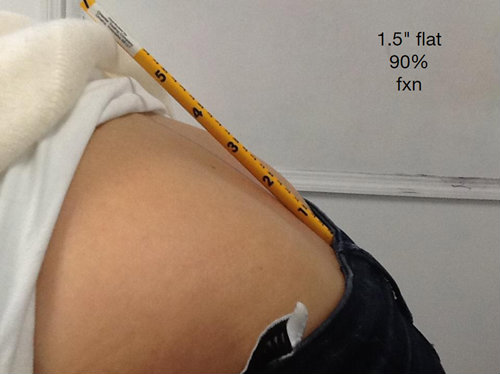 A C-grade low back – 75% function (fxn) – Notice the pencil is flat for 3″:
A C-grade low back – 75% function (fxn) – Notice the pencil is flat for 3″: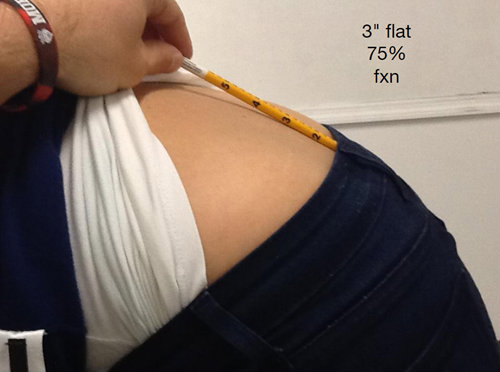
Or a D-grade low back – 65% function (fxn) – Notice the pencil is flat for 4.5″: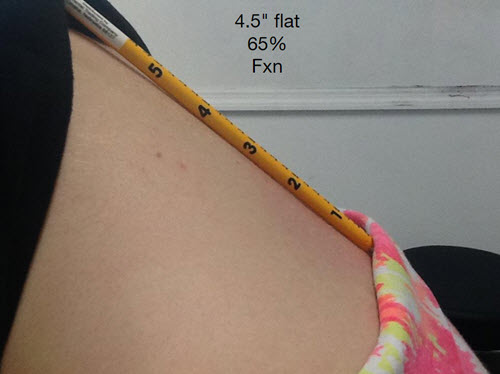
Or do you have a major fail – 40% function (fxn) – Notice the space under the pencil: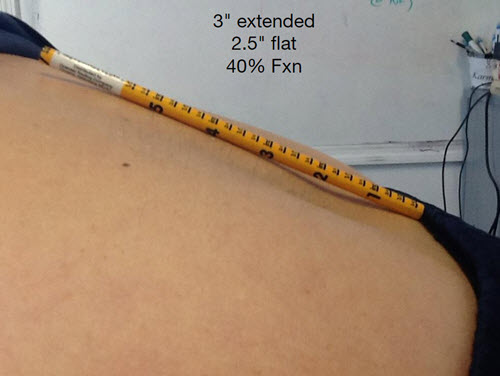
Then, if you do the Touch Your Toes Test and the speed of your movedment is Yellow-Lighted, then you can be confident you have a disc problem (and NOT Piriformis Syndrome). You can be CERTAIN you have a disc problem if you have pain or tightness in the MIDDLE of the range of motion that gets better as you get to your end range.
Are there any other tests you can do?
- An MRI can confirm low back disc involvement.
2 Piriformis Syndrome Treatments That Work
Your head may be spinning a bit right now.
Diagnosing pain cases that have lasted more than 6 months and have been failed by multiple doctors requires deeper thinking.
That’s why the very first sentence of this post tried to get you off of this page. If you weren’t ready to use your head, you wouldn’t have spent the mental energy to try to figure out what your problem really is.
Now, you should have confidence whether you have Piriformis Syndrome or not.
If you do have Piriformis Syndrome, there are only 2 treatments that work to remove the adhesion from your sciatic nerve and the hip external rotators.
There is some research stating that a steroid injection works for 50% of patients. If this worked, there was either no or minimal adhesion. If you’re not able to try Piriformis Syndrome Treatment #1 below, I’d do this as the next step before trying Piriformis Syndrome Treatment #2.
Piriformis Syndrome Treatment #1: Get Your Adhesion Removed With Manual Therapy
Healthcare standards universally say to treat conservatively (without getting cut open) before invasively (getting cut open).
This applies here.
A skilled adhesion removal specialist like an Adhesion Release Methods provider can feel where the sciatic nerve is stuck with only his/her hands.
Then, he can remove that adhesion with the help of an assistant.
Below is a live case study with a young professional dancer with a tighter right hamstring than the left. He’s been stretching for years, not seemign to make a dent in his flexibility. The great thing about this treatment is, 3 passes, and 48 hours after the treatment, Ray said:
I’m still tighter in my left hamstring now! Will it stay this way?
I replied, “Of course. There’s less adhesion in your right hip now!”
The results are often immediate, with significant relief happening within 5 treatments.
Piriformis Syndrome Treatment #2: Get Your Adhesion Removed With Surgery
Or, you can go straight towards getting cut open.
Interestingly, a common cause of Piriformis Syndrome is previous piriformis release through a steroid injection.(Source – 18:00)
TAKE ACTION NOW: Find a Specialist
Regardless of which Piriformis Syndrome treatment you want, you’ll need to find a specialist as there aren’t many doctors doing this type of work.
To find a doctor/provider to release the adhesion (treatment #1) with his hands, I recommend finding a provider on Adhesion Release Methods.
If you’ve already tried conservative care with an Integrative Diagnosis provider, I’d contact one of two doctors:
Dr. Hal Martin, lead author of The Endoscopic Treatment of Sciatic Nerve Entrapment/Deep Gluteal Syndrome.
Address: Oklahoma Sports Science & Orthopaedics, 6205 N Santa Fe, Ste 200, Oklahoma City, OK 73118, U.S.A.
Dr. Shane Tipton, lead author of Arthroscopic Decompression of Greater Trochanteric Sciatic Nerve Impingement.
Address: Department of Orthopaedics, Wake Forest School of Medicine, Winston Salem, North Carolina, U.S.A.
If you can’t get to Oklahoma or North Carolina, these doctors would likely know the closest surgeon to you who can help you with your pain.
 If you have questions about your butt pain, please answer all of the questions below about your pain and I can help steer you in the right direction. If you don’t give me all of the answers, I’ll reply and ask you to give me ALL of the answers.
If you have questions about your butt pain, please answer all of the questions below about your pain and I can help steer you in the right direction. If you don’t give me all of the answers, I’ll reply and ask you to give me ALL of the answers.
- How old are you?
- Any trauma to the area?
- Where is the pain?
- Describe what the pain feels like.
- What makes it worse?
- What makes it better?
- What is your range for the Hamstring Stretch Test?
- What is your range for the Pencil Test?
- What is your range for the Touch Your Toes Test?


Sarah Cummings
Posted at 10:35h, 01 OctoberGreat post! Thanks for sharing this information. Such a big help!
Dr. Chris
Posted at 13:15h, 01 October: ) Happy to help.
Sana thahane
Posted at 18:51h, 07 MarchHi Dr Chris I need help
Dr. Chris
Posted at 10:58h, 12 AprilI’m here for you. What kind of help?
Jane L Siebert
Posted at 18:22h, 31 JulyHi Dr. Chris- I’m needing help with my pain!! Is there a specialist in the Springfield MO area? Have been suffering for 3 1/2 years with butt pain and upper leg pain/hip pain. But went 2 years without any kind of treatment and have spent the last year and a half doing various physical therapy treatment exercises, heat and stem, myo, ART, massage, etc. used to be a runner but now can only walk slowly but it still causes pain . Many of my symptoms and scenarios are similar to the ones addressed in your article and of people responding to you. It hurts when I have to bend over and pick up something or going upstairs etc. Wanting to thing to avoid surgery and steroid injections . I feel like I have the adhesions to the nerve like you mentioned earlier. What other test or examinations do I need ? Wondering about an MRI ?
Dr. Chris
Posted at 23:00h, 02 AugustGo see Dr. Matt. One of the Top 3 Chronic Pain Doctors in the world, right in St. Louis.
He’ll take care of you.
https://www.precisionhealthstl.com/
Ginger Berry
Posted at 19:11h, 21 MarchI suffered 3 plus years before back surgery, 2 level fussion and laminectomy. I had bone on bone rubbing , disk were gone. It’s been 1 year since surgery, doing better in some ways, but still having sciatic pain in buttocks down both legs into the forefoot. Tried just about everything. A pain dr before surgery, gave injections into both periformis muscles and pain completely stopped for 3 hrs all the way down into the toes.
Would like to try removing adhesions manually. Tried your online address and did not have success!!! Please send me info where I can go and try this. I’m in oklahoma, but will go almost anywhere to try this!!
Thank You!!
Dr. Chris
Posted at 10:58h, 12 AprilHi Ginger, sorry for delay. I’d go to Thrive Spine and Sport in Iowa. Check out their reviews. DOn’t waste your time with anyone else.
Rhys Myors
Posted at 00:52h, 24 AprilHi Dr Chris,
I’m a Marathon runner, was averaging 60-70m per week
38yo
Pain in the centre of left buttock, doesn’t radiate down leg, but my butt gets numb.
Left side is significantly tighter than right (hamstrings, hips)
Flexibility is ok about 70deg in the left hamstring.
Symptoms came in about 2months ago, after a tempo run.
Have been getting regular PT (not really impressed) stretching 3-4 times a day, lots of rolling and lacrosse ball in my butt. Doing strengthening of my hips as well.
Pain is pretty much no change. Some days no pain, some days really sore.
Haven’t run in over a month
Getting quite frustrated, any advice on someone I could go see in Northern Virginia (I live in Alexandria and work in Arlington)
Thanks
Dr. Chris
Posted at 10:26h, 24 AprilHi Rhys, based on what you shared, Im not clear on whether it’s actual piriformis syndrome or a disc problem shooting down. If you’ve done more than 5 treatments without permanent relief in any way, I’d see a new doctor or therapist. 5 visits is the expectation for relief. I don’t know anyone who does adhesion work in Virginia – none of my colleagues are there. You can try some people and see if they help.
Parvez s. Shaikh
Posted at 16:06h, 02 MayHi Doctor, I am parvez from India, is suffering from piriform is syndrome for last 10 years, it gets worse at night while in bed, need to massage for 1 hour to get relief, there is no permanent cure, will be very happy if you help me get rid of this pain from right buttock, back middle of thigh, back middle if calf, my email id is shaikhp2001@gmail.com
Will be very happy if you help guide me to relieve this severe pain
Dr. Chris
Posted at 16:58h, 02 MayHi Parvez, unfortunately the problem requires treatment like one of the two above. I wouldn’t be able to give you treatment virtually. I recommend planning on travelling to someone who can help you fix the problem.
Lee Miller
Posted at 02:45h, 07 May1. How old are you? 48
2. Any trauma to the area? No
3. Where is the pain? Butt, side/front low leg, outer/top of foot.
4. Describe what the pain feels like. Electric nail gun
5. What makes it worse? Standing, walking, becomes worse if carrying anything
6. What makes it better? Hard constant pressure on outside low leg or hard constant pressure on glutes
7. What is your range for the Hamstring Stretch Test? Farther than the dancer’s range in your video at 113 degrees
8. What is your range for the Pencil Test? 90% function
9. What is your range for the Touch Your Toes Test? My palms are flat on the floor
My flexibility makes me appear normal but the pain at level 8 day/night for more than 12 months
Dr. Chris
Posted at 10:02h, 07 MayHi Lee, you definitely have a disc pathology in the low back. It’s not big or significant enough to affect your ranges, but it obviously affecting your L5 and S1 nerve roots (google “Lumbar dermatomes” to see which nerve areas are affected). If you get an MRI, it might be some type of extrusion. I recommend getting one to see what your discs look like.
PAUL BASILE
Posted at 17:38h, 18 Maydr chris…..WOW real solutions for my seemingly bilateral Piriformis issues. i can’t make it to Denville unless i coordinate a visit to my old stomping grounds in River Edge or Cliffside Park, so can you recommend someone here in Bend OR (or anywhere in OR) that can do this work?
Dr. Chris
Posted at 20:27h, 18 MayHi Paul, fellow New Jerseyan. We don’t have an Integrative Diagnosis Doctors in OR. There’s one in CA (mydrcohen.com). He’s the closest to you. I recommend going to see him. I travel from NJ to Boston or Chicago once/month for my own treatments.
Brigitte Biel
Posted at 14:59h, 19 MayI have an adhesion problem in my gluteus muscle(s) and I would like advice how to get rid if them. is there a specialist in the UK who can help?
Dr. Chris
Posted at 00:09h, 20 MayHi Bridgitte, there are no specialists in UK. Only US and Australia at this time.
Chris Crowell
Posted at 15:31h, 19 MayAnswers to your 10 questions below.
I’ve had piriformis syndrome for approximately 2 years. I’ve studied it in great depth as the pain is debilitating and I need to fix it. I’ve been to at least 6 physical therapists as well as the Rothman clinic in Philadelphia. The physical therapist was recommended by Rothman and while they were good unfortunately they were not that familiar with this condition. I’ve followed their last advice which was to strengthen the area with mild exercise. That’s improved the condition by about 30% but the improvement has plateaued.
I was in the process of considering Extracorporeal shockwave treatment. I’ve heard of good results from a piriformis blog I’m on but I have reservations. I’ve heard of the nerve adhesion issue in the items I’ve read but the stretches recommended haven’t helped. To your point I may be beyond a stretching solution.
As an FYI, I got this by overstreching my piriformis. I was having some back pain and someone recommended this stretch. It worked so well I continued to use the stretch daily for an extended period. However I slowly developed a pain in my buttocks which progressed to where I am today.
I’m in a great need of help.. I live in Dover Delaware and would gladly travel to your clinic if you could help. Looking for your advice. Thanks. Answers below:
Age -64
Trauma – no
Pain – buttocks follows an exact path of piriformis. Radiates down back of leg when pinching sciatica.
Description- extreme in the morning, slightly better during the day returning at night and only slightly better during sleep.
Makes it worse- extended walking
Makes it better- surprisingly massaging with a roller. However the relief is very temporary.
Hamstring test – performed at last PT session. I damned near jumped off the table. Incredible piriformis pain
Pencil test- I’m not sure exactly where but I’m in the ok range..
Hope you may be able to help. Also interested if you’ve heard of shockwave therapy.
Thanks
Dr. Chris
Posted at 00:12h, 20 MayHi Chris, hard to say whether it’s more disc or piriformis. We’d have to dive into the details with an exam. I recommend you pull a Melissa (https://www.youtube.com/watch?v=FG80em9dh38&t=132s) and drive up here – we’d do a consult, exam, and if we come up with a diagnosis that includes adhesion, treatment, and see how it goes. At minimum, we’d diagnose it so you know what you’re dealing with.
Ildiko Toth
Posted at 20:18h, 05 OctoberHi Chris,
I have read your lines here on barefootrehab.com and also on another piriformis blog. My story and symptons (ovestretch and then developing piriformis and sciatica) is strikingly similar to yours. I was wondering how much adhesion removal by manual ontegrative therapy finally helped you. How are you doing these days? Have you managed to resolve the problem? I am desperate to avoid surgery. Please let me know what else helped you.
Ildi
Drew Baxter
Posted at 04:23h, 29 MayHi Chris,
Can you please tell me where the Australian specialists are who can perform this treatment?
Thanks!
Drew
Dr. Chris
Posted at 10:56h, 29 Mayhttps://integrativediagnosis.com/find-an-id-provider/
Drew Baxter
Posted at 00:28h, 30 MayTHank you. Unfortunately, I’m in Melbourne, they are only in Sydney and Perth..
Dr. Chris
Posted at 07:46h, 01 JuneYou’re welcome, yes, that is unfortunate. I recommend doing what you have to do to see one of these specialists. I wouldn’t waste my time with local doctors unless you need to in order to see for yourself that you need an ID Specialist.
PETRINA SKUTTA
Posted at 19:47h, 05 JuneI’ve had a herniated disc since Jan 2019 and as a result have piriformis pain. I have been seen by a chiropractor, then did physical therapy, then tried two treatments of PRP and therapeutic massage and am still in pain. I live in south Florida by Boca Raton and am wondering if you could recommend anyone I can see down here please. Thank you
Dr. Chris
Posted at 10:19h, 06 JuneHi Petrina, 2 doctors do this in Florida. Peak Soft Tissue and Veracity Soft Tissue.
Michelle Lipoma
Posted at 03:19h, 06 JuneHi,
My 17 y.o son has been having pain in his lower back/right buttock area. He complains of “feeling tight” and running makes the pain unbearable. He will usually get relief from stretching or deep tissue massage but it doesn’t last. He is a baseball player and unable to play at this time. He had a MRI of his lower back which was negative and is currently in PT. He has had a steroid shot which had minimal effects. We live in Baton Rouge,La. His ortho mentioned a performs muscle issue and suggested resting for 28 days which he did. But the pain has returned with minimal activity such as batting. Any suggestions would be appreciated
Dr. Chris
Posted at 10:21h, 06 JuneHi Michelle, do the hamstring stretch test and pencil test above to get a rough idea of where the problem is. It’s hard to say based on this history if his sciatic nerve is entrapped at the butt cheek or if it’s a disc. I believe Precision Health Group in St. Louis is closest provider to you. They have people who travel across the country for their care and highly recommend not wasting time or money with other providers.
Talya
Posted at 11:08h, 10 MarchHi Michelle, I’m having pain of high similarity to your son’s pain (as it was described by you). Before it started I was getting ready for a half marathon, now I can’t run at all, Physiotherapy didn’t help me. Did you find any helpful and reliable treatment for your son? maybe it could be useful for my case as well.
Thanks in advance
Dr. Chris
Posted at 12:13h, 10 MarchHi Talya, what works for you will depend largely on all of the variables contributing to your pain. When iti comes to chronic pain, blanket treatments are very dangerous as they waste time and money. I recommend getting a very precise diagnosis – then, treatment WILL work.
Carolina S
Posted at 12:33h, 15 JulyHi Chris,
I found your website as I have been suffering from what has been diagnosed as Piriformis Syndrome in my left side for over 10 months. Since it started, the pain has gotten better, but has basically plateaued, so I do not feel that I am necessarily getting better, but definitely not getting worse. I got an MRI on my lower back and hips, and everything was normal. There is no disc issues causing the sciatic nerve pain. The doctor has told me it is most likely spasms in the piriformis or possibly hamstring that is causing the pain. I have tried just about everything (swimming, pilates, yoga, PT, massage therapy, cupping therapy, myofascial release therapy, foam rolling, stretching, hot/cold therapy, electrical stimulation therapy, etc.), but I can’t seem to fix this problem. I’ll provide all of my details below as requested. Thank you in advance.
How old are you? 29
Any trauma to the area? About 10 months ago, I did a high-intensity fitness class where we held a hip bridge for 5 minutes and the next day I ran 5 km in very hot weather, and the next day, I could barely walk or sit in a chair. It was painful to walk or sit, the only relief I had was laying down. I suspect that something in this fitness class or from the run caused some sort of injury. I stopped doing exercise for some time and just focused on swimming and I went to PT for a few sessions. They told me it was a hamstring injury that the muscle had gotten all twisted up inside and they needed to unwind/release it, but I wasn’t convinced with the diagnosis because PT did not help me very much, it almost felt worse after PT. I found relief by starting to do yoga again and I do yoga regularly (2-3 times a week, Bikram and regular). I slowly began to incorporate other fitness (weightlifting, spinning) into my routine again. I never felt pain when doing any exercise. I always warm-up and stretch before and after any exercise.
Where is the pain? The pain is only when I sit for more than 5-10 minutes. It starts in my hamstring area and radiates down through my calf. Sometimes I also feel pain in my piriformis area when sitting for too long.
Describe what the pain feels like. It’s an uncomfortable pain, not a sharp pain but more of just a dull pain that is incessant. When I stand up and walk about or stretch, it goes away. But as soon as I sit down again for an extended period of time, it starts up again. I can also feel my muscle twitching sometimes when I sit for too long.
What makes it worse? Sitting in a chair. Some chairs are better than others. For example, sitting in a car doesn’t bother it so much because the chair doesn’t touch the hamstring directly. Or when sitting on a couch that is low to the ground that doesn’t make contact with the hamstring, it doesn’t hurt. But if it is a high couch where it is pressing up against my hamstring, I can start to feel the pain pretty soon.
What makes it better? Laying down, extending my legs, standing up, stretching.
What is your range for the Hamstring Stretch Test? Full range, 90 degrees, no pain
What is your range for the Pencil Test? 3 cm (or 1.2 inches) before there is space
What is your range for the Touch Your Toes Test? Pass. Second knuckles touching the ground effortlessly. No pain, just feels like a regular stretch.
Dr. Chris
Posted at 00:36h, 18 JulyHi Carolina, you definitely don’t have piriformis syndrome with 90 degrees of hamstring stretch range. Even though your MRI is clean, it’s most likely a disc issue “referring” the pain to the piriformis area and also causing hamstring/calf symptoms. I’d try finding a Manual Adhesion Release doctor wherever you live to help it. In the meantime, I’d take as much stress off your low back as you can.
Kane
Posted at 17:43h, 31 JulyHi Dr. Chris,
I just read your post and among the hundreds of post and research that I have read this post really made a point. I have been suffering for a back injury for more than 8 months. I’ve been to several doctors you name it you got it physical therapist, neurologist, etc they cant really tell what kind of pain I’m experiencing. I have CT scan than MRI which I think MRI can really tell what’s happening inside me. I had to say the doctors in the Philippines is not really that cool. Anyway I think I diagnose my self haha I think I have a Piriformis syndrome I am just not sure how did I get it. Maybe prolong hours of sitting at work, Too much exercise, I cant think of anything. Few months ago I was able to walk properly without any pain radiating from my buttock to inner calf. I didn’t want to have an operation because I think If I will undergo through that I would loose some parts inside me that will make me more inable to do things. That is just me not offending anyone else. I tried physical therapy session but it did do better on me. I researched some few ways on how I can be better so I saw this Chiropractic Doctor in Manila and I had several sessions with him. Thank God after my fourth session one day I started to notice that the radiating pain is gone. The reason why I am writing now in your post is a month ago I felt a lower back pain again. I dont know why I felt it again but I have been very careful about how I would move around not carrying heavy things regular stretching. I am observing myself to see if the radiating sharp pain will ever go back. Do you think I need manual adjustments again to ease the pain Im going through. Thank you and more power!
Dr. Chris
Posted at 22:58h, 02 AugustHi Kane, I’m sorry for your troubles. The fact is, PAIN = too much stress on some body part. Even if you did a little bit, your body is saying “that little bit” was too much. If I were you, I’d find the best myofascial therapist I could find. This is your best bet to getting better.
Sarahi Rojas Reyes
Posted at 05:22h, 08 AugustIs feeling something hard in glute a sign Piriformis Syndrome.
I cant sit on the toilet or in a hard chat because i feel I’m sitting on something hard on my right glute. + I have all the other symptoms
Dr. Chris
Posted at 10:59h, 08 AugustThe symptoms you describe can be “piriformis syndrome” or a “disc”. You need more data.
Ben Hall
Posted at 13:46h, 10 AugustHi Chris. Can you recommend anyone in Atlanta, or Georgia to see for stubborn Piriformis Syndrome? I’ve tried PT, Chiro and massage with minimal improvement.
Dr. Chris
Posted at 11:20h, 20 SeptemberHi Ben, check it out here. There are providers in FL or South Carolina I believe. https://integrativediagnosis.com/find-an-id-provider/
Katy
Posted at 17:08h, 19 SeptemberHow old are you? 33
Any trauma to the area? No
Where is the pain? Low back, both glutes which radiates down mostly the outer left leg to the ankle
Describe what the pain feels like. Burning, deep ache
What makes it worse? Sitting for long periods and standing
What makes it better? Laying down, stretching the piriformis and hamstrings
What is your range for the Hamstring Stretch Test? Good
What is your range for the Pencil Test? C grade
What is your range for the Touch Your Toes Test? Fail-high risk
Dr. Chris
Posted at 11:21h, 20 SeptemberHi Katy, sounds like a disc. Focus any treatment you get there on low back.
Matthew Dwight
Posted at 20:25h, 16 OctoberHi Dr. Chris,
My wife has been to 2 PTs, 2 Chiros, 1 pain management specialist and has had 1 injection done directly into the piriformis muscle, not to mention almost 8 months of PT, chiropractic appointments, MRIs, X-rays (both came up clean every time), stretching, and isolated strength training. She’s been dealing with pain for 2 years and we finally know for a fact it’s Piriformis Syndrome, as concluded by all the PTs, Chiropractors, the pain management specialist, and my wife. We’re here in Dallas, TX and after looking for doctors on https://integrativediagnosis.com/find-an-id-provider/ the closest I’ve been able to find is in Denver or St. Louis. My first question is, is it worth going to see one of these specialist or do you know someone in TX that might be closer? My second question is, would flying or driving to see one of these specialist and then returning home undo what the specialist did? I’m worried the length of time my wife would be sitting will cause more damage or discomfort. Thank you in advance for your help and your very educational article.
How old are you? She’s 26 and has a lean body type.
Any trauma to the area? Possibly? Not sure, She used to snowboard and now she sits all day at a desk (I think that counts as trauma)
Where is the pain? In her butt and lower back, but mostly isolated to her right butt cheek.
Describe what the pain feels like. She’d be able to tell you better than me.
What makes it worse? Sitting for long periods of time, walking a lot, sometimes lying flat on her back
What makes it better? she does a certain stretch that seems to help. Not sure how to describe it.
What is your range for the Hamstring Stretch Test? good range, pain is isolated to right butt cheek
What is your range for the Pencil Test? different PTs, different results but best result at the end of several months of PT was around 85%
What is your range for the Touch Your Toes Test? By the end of PT she could just touch her toes
Dr. Chris
Posted at 00:35h, 28 JanuaryHi Matt, so sorry for delay. Comments were going to my spam. Sounds like a disc. Did she find an answer yet. I highly recommend going to Precision Health Group in St. Louis. He’s the 2nd best doctor in U.S. at fixing chronic pain. Gets people flying in all of the time. I’ll be checking comments so I can support you if you have any questions.
Matthew Dwight
Posted at 15:58h, 30 JanuaryNo worries, I appreciate the reply. We haven’t found any solutions yet, we gave up on Physical Therapy since her insurance wasn’t covering it and they honestly didn’t have a clue after almost a year of going. I’ll talk to her about making a trip to St. Louis. Her brother lives there anyways so maybe we can combine the trip into one. Some one needs to open an office further south!
We did find out recently that she does have a small tear in her hip flexor (probably from falling while snowboarding according to the Dr.s) but they don’t think it’s related to the pain. Since my first comment she’s had two more MRIs (right hip and lumbar spine), 2 more x-rays (lumbar spine and pelvic), and and an acetabular labrum injection, both injections helped temporarily but the pain moved toward one side of her sacrum. She did find a stretch that helps, its called the piriformis figure 4, a foam roller also provides some relief, clam shells and hamstring stretches help a little too. She’s taken up yoga to try and help but it doesn’t seem to be helping much and certain stretches light it up and piss it off.
Dr. Chris
Posted at 02:37h, 31 JanuarySounds like you’re doing good stuff. I hope it gets her relief. If it doesn’t, please make it to St. Louis. : ) Here for you. <3
Daksha Patel
Posted at 18:03h, 18 OctoberThis really helps. any doctors in Ventura County California?
Dr. Chris
Posted at 00:34h, 28 JanuaryOnly doc in CA. https://www.facebook.com/mydrcohen/
Theresa Schrock
Posted at 22:02h, 21 OctoberHi Dr Chris,
I have been having pain in the left side deep in the butt area, and side hip, an occasional back pain not too often and have seen a Chiropractor for ART about 8 sessions each, and now seeing a PT that specializes in running, about 8 sessions so far, with dry needling and scraping so far. It is getting better slowly but not completely gone. I know the next time I go running or exercise it is going to flare up again, Can you recommend someone here in the Denver, CO area?
How old are you? 49
Any trauma to the area? no
Where is the pain? left butt (deep), side hip and sometimes hip flexor
Describe what the pain feels like. Feels like a chronic nagging pain, When I am sitting, I feel like I am sitting on a rock.
What makes it worse? Distance running, Laying on the side, pain with specific exercises, such as side shuffles, Split stance lunges, jump squats, jump lunges, side plank toe touches.
What makes it better? nothing so far.
What is your range for the Hamstring Stretch Test? good
What is your range for the Pencil Test? about 2-3 inches
What is your range for the Touch Your Toes Test? green light, no issues
Dr. Chris
Posted at 00:35h, 28 JanuaryHi Theresa! Novo Soft Tissue in Denver. Sounds like a disc. Dr. King is amazing. I wouldn’t see anyone else.
Artjom Svjatickis
Posted at 02:41h, 25 OctoberDr.Chris please tell me someone i can go to to treat this in southern california. Im in excruciating pain cant do anything, i cant find a position where i am not in pain in my left buttock. Its been manageable, but i woke up this morning and i cant do anything without 10/10 pain. Please help i dont want surgery
Dr. Chris
Posted at 00:35h, 28 JanuaryHi Artjom! The only doc in CA who is certified in removing adhesion is https://www.facebook.com/mydrcohen/
Janice Mirch
Posted at 02:26h, 26 OctoberHi Dr Chris, can you recommend a specialist in Chicago IL?
Dr. Chris
Posted at 00:36h, 28 JanuaryYou’re lucky. Functional Pain Relief is one of top 3 doctors in the U.S.! Go see them!
Fadi
Posted at 12:51h, 12 NovemberHi,
I’ve been suffering for more than 7 months already, with each time I start feeling better something happens (sometimes just a sneeze) and its all full 10/10 pain all again.
I really liked your post and I wonder if you recommend anyone who can perform this treatment in Israel or even close to Israel (Europe), because it’s really hard and expensive to come to USA, and I’m really desperate.
Please help,
Thanks
Dr. Chris
Posted at 00:36h, 28 JanuaryHi Fadi, I’m sorry, this is still a very new technique. We don’t have anyone outisde of US and Australia.
Athena
Posted at 23:46h, 23 NovemberI hurt my back 3 years ago, but have been to PT and accupunture, and other various treatments. I have had multiple mri s and my discs look pretty good. According to docs – I’m non surgical. I have sciatic pain down my left leg all the way into my foot. My right foot has a fullness feeling to it. Both feet have a squeezing feeling around the ankles. I have had 2 steroid shots in my Piriformis and it helped, but now it is back. Had 2 shots on the right and it did nothing. From all I have read it seems to me that my sciatic is irritated but not sure why. I live in Wisconsin. Any suggestions would be helpful
Dr. Chris
Posted at 00:37h, 28 JanuaryIt’s defnitely a disc. The chances of having bilateral piriformis syndrome is NOT likely at all. Check out the ID website? I believe tihere is a newer doc in Wisconsin specializing in removing adhesion.
Chris
Posted at 16:45h, 25 NovemberI’ve been having pain in the exact same area as the man you’re treating in this video. I’ve been prescribed a steroid, completed a session of ART, tried strength training exercises, and have recently been doing PT – the pain has continued to last for going on 5-6 months now. Oftentimes the pain will refer to the top of the hamstring, right under my butt cheek. All the symptoms point to piriformis syndrome. What would you suggest as far as next steps? I live in DE and I doubt there’s a provider here that is familiar with the treatment you performed – would it make sense to schedule an appt with your office since it’s within somewhat manageable driving distance? Appreciate any help!
Dr. Chris
Posted at 00:38h, 28 JanuaryHi Chris! So sorry it’s stilll hurting. ART won’t get it. We stopped referring to ART providers across US years ago. Yes, I recommend calling us to see if you’re a candidiate. We just had a patient come from Delaware last summer. Got 50% relief in 4 treatments. 862 205 4847
Joe Thompsn
Posted at 18:18h, 27 NovemberKnow any Dr. in the Charleston, SC area who would be good for Piriformus Syndrome?
Dr. Chris
Posted at 00:39h, 28 JanuaryHi Joe! I believe there are a couple of newer docs in Charleston. Check out the website: https://integrativediagnosis.com/find-an-id-provider/
Kristina Kozak
Posted at 00:46h, 12 DecemberDo you have the names of drs closest to New Jersey that perform the manual therapy.
Dr. Chris
Posted at 00:39h, 28 JanuaryLOL – we just met you Kristina!
Savannah Lehman
Posted at 20:40h, 24 JanuaryHi- Wondering if you could offer any insight into my pain. Started when I was 3 months pregnant back in 2016, went away after delivery, came back in 2018 3 months into my 2nd pregnancy and has not gone away since. I’ve tried everything – PT, chiro, steroid injections, acupuncture, myofascial, PRP, etc and the pain is still there in my right glue [piriformis is where it seems to be centered]. No pain radiating down the leg or back at all.
1. 34
2. No trauma, but pain started during pregnancy so perhaps that’s a cause/catalyst
3. Pain in right piriformis/center of butt cheek
4. Pain feels throbbing at times, and is hard to ignore when doing simple daily tasks
5. Worse when sitting for long periods, laying down, squatting/lunges, sneezing/coughing sometimes
6. Nothing really…shifting weight onto left side helps
7. In the GOOD range
8. In the OKAY range
9. No pain, feels like a stretch
I’m in the Harrisburg PA area and started seeing someone who practices P-DTR therapy- too early to see if it’s working and I still have pain. Any help would be AMAZING!! I’ve been an athlete my whole life and haven’t been able to exercise for 6+ months, it’s so awful!! Thank you!
Dr. Chris
Posted at 00:40h, 28 JanuaryHi Savannah! Sounds like a disc. Piriformis syndrome wouldn’t get worse with increased weight of pregnancy. We are the closest adhesion specialist to Harrisburg. We get people from far out of state all the time. Not sure if it’s bad enough to make the trip? We’re here for you.
Savannah Lehman
Posted at 18:31h, 28 JanuaryI’m not sure if it got WORSE per se, but it definitely started during pregnancy both times. I had a lumbar spine MRI done which showed a slight bulge/tear in my L4 L5 if that is helpful. Yes it’s definitely bad enough for me to go anywhere that can help, What would you suggest? What do you guys do, and have you seen this type of issue before??
Dr. Chris
Posted at 22:34h, 28 JanuaryHi Savannah, the fact that started during pregancy says that the increased stress/load (from the baby) along with loose ligament and hormone issues is the VERY likely cause. I’d suggest coming to see us. You can try local PA doctors – however, I’ve found this to be a waste of time when pain is chronic.
Yes, we see pregnant women all the time. Here’s a video of us treating one : )
https://youtu.be/mVmVEJL1h0U
Ryan
Posted at 13:51h, 11 FebruaryHey great article, any manual adhesion doctors around Long Island NY? I had a s1/l5 discectomy for my herniations and I’ve still had horrible piriformis syndrome for about 6 months now. No matter what I do it flares up and makes it worse! PT massage therapists etc.. I’ve had more luck just resting and slow walking. I am going crazy reading the amount of posts to just “stretch” appreciate the help.
Dr. Chris
Posted at 20:16h, 11 FebruaryTY Ryan. We’re the closest. We have many patients come from Long Island, just had one come from Long Beach today. Yeah, don’t bother stretching.
This is why we had a patient even drive up from Texas. https://youtu.be/FG80em9dh38
Frustrated? Piriformis Syndrome Treatment That Works When Your Pain Has Lasted Longer Than 6 Months – piriformis syndrome
Posted at 09:05h, 08 March[…] Source […]
Lee Cavallo
Posted at 03:45h, 15 AprilHello! I have been suffering from Piriformis syndrome for 6 plus months. Pain in the front right of my shin that goes down to my toes. Sometimes feel it in the back of my leg. Had a lower back MRI and a lower leg MRI and both are clean.
Do you know any specialists in San Diego, CA? Desperate to get something to work. Have tried active release therapy with no results, as well as every piriformis syndrome stretch under the sun. My next course of action is to get a cortisone shot in the muscle to relieve some pain.
Dr. Chris
Posted at 16:16h, 20 AprilThis is 99% NOT pirirformis syndrome. The sciatic nerve, which is the nerve that gets caught under the piriformis, rarely has a branch that goes to anterior shin. It’s way more common to be a low back disc problem pushing on the nerve roots – usually L5 nerve root.
Do the cat-cow test – does it provoke these symptoms?
If not, lie on your back and stretch your hamstring til you feel ANY moderate symptom. Then point your toes. Did the shin get provoked?
Just because the low back MRI is clean doesn’t mean it’s not a low back issue as they’re not 100% Perfect.
The only adhesion doctor in CA is Dr. Cohen here. You may have to travel. https://www.mydrcohen.com/
Joy Salako
Posted at 01:05h, 06 MayDr. Chris,
Your help would be greatly appreciated. I have been suffering for over 6 months from what the doctor has diagnosed as piriformis. Over time, it has gradually progressed to the point that I am now limping. I have a sharp pain in my butt, that resonates down to my calf. I also feel a numbness in my pinky toe. It’s gotten to the point where its extremely uncomfortable to do anything. Yoga, walking, and physical therapy have only made things worse. I get small relief after massaging the area, but that is short lived. I live in the OKC area. I wasn’t able to find a physician using the Integrative Diagnosis search. PLEASE, is there anyone you can recommend in the OKC area, preferably one that offers the manual relief option? Thank you.
Joy Salako
Posted at 01:05h, 06 MayI’d like to add that I am now 2 months pregnant, so that makes things all the more worse.
Dr. Chris
Posted at 16:16h, 06 MayHi Joy, I’m sorry to hear all of this. Like we mentioned above, most people who have been diagnosed with “piriformis syndrome” actually have a disc problem. Have you had an MRI of the low back?
You may have to travel if you want an Integrative Diagnosis doctor to see you. There is one in Iowa and one in St. Louis.
The other option is we have a virtual Chronic Pain program (2-3 months) with guaranteed relief or your money back. LMK your thoughts.
Melinda
Posted at 17:54h, 01 JuneI have been diagnosed with Piriformis Syndrome. It’s been 7 months and I have done all the stretches and exercises given to me and it hasn’t gotten any better. In fact, the sciatica has gotten worse. Is there anyone near Riverside, California that can help me?
Dr. Chris
Posted at 22:44h, 01 JuneHi Melinda, I’m sorry to hear this. If it’s a disc problem or adhesion, stretches and exercises won’t help. The only person who is certified to remove adhesion in California is Cohen Soft Tissue. Not sure where he is though.
Alex
Posted at 19:22h, 14 JuneHI Dr. Chris,
1. How old are you? 51
2. Any trauma to the area? No
3. Where is the pain? left butt cheek. Had it for 5-7 years,
4. Describe what the pain feels like. Soreness with small electric current running down my leg, cant barely sleep, the electric shock sensation wakes me up repeatedly.
5. What makes it worse? sitting for extended period of time. I’m a financial trader for living so I sit long hours. Running also, which I’ve tried avoid doing for couple of years.
6. What makes it better? standing up or laying on side after sitting long hours but relief only last a few mins
7. What is your range for the Hamstring Stretch Test? 90 degrees
8. What is your range for the Pencil Test? 90% function
9. What is your range for the Touch Your Toes Test? I slow down 2-3 inches from floor but can’t touch floor.
I’ve never had excruciating pain but the soreness and electric shocks current hasn’t left sleep comfortable for several years now, something I can only sleep 1-2 hours/night,
I currently reside in the San Diego, CA area, Please point me in the right direction, Thank you
Dr. Chris
Posted at 21:01h, 16 JuneHi Alex, sounds like it’s probably the disc based on Hamstring Stretch being so good. If it were truly a sciatic nerve entrapment at the piriformis, it wouldn’t be so good. My only colleague in CA is Cohen Soft Tissue. Not near San Diego though. I recommend traveling as local massage providers won’t likely be able to help.
Laura Kurry
Posted at 16:42h, 28 AugustHi Chris,
I’ve become desperate to find help with my hip/leg pain and began looking at blogs and found this Barefoot Rehab discussion. Just looking at your site makes me feel better knowing I’m not alone (or crazy)! I live in Birmingham, AL and would consider myself very active and fit. Since January of 2020, I’ve had had 4 spinal blocks, (epidural, L4-5 nerve block, sacrum and Piriformis, with no relief). I’ve taken a Medrol Dose Pack, Flexeril, Neurontin, purchased a TENS Unit and used to the point it didn’t really affect me anymore. I’ve had MRI’s to right hip, lumbar spine and pelvis that showed no significant findings. EMG Interpretation & Conclusions showed, “evidence consistent with irritation of the peroneal portion of the sciatic nerve on the right. These findings could also be consistent with irritation of the L5 nerve root though normal findings at the flexor digitorum longus muscle makes this less likely. There was no evidence of acute radiculopathy, generalized neuropathy or myopathy as a major factor to the patient’s complaints.” Whatever that means!!!
I’m being sent to have another Piriformis block next week from another provider, and if no relief, will receive a Myelogram. I’m currently working with a physical therapist who is trying to manipulate the sciatic nerve and helping me with adductor and core muscle strengthening exercises. I believe in my therapist and practice exercises daily with therapy 2 x’s per week.
I’ve been coping with pain for 8 months and hoping/praying you can help advise me.
How old are you? 58 years young
Any trauma to the area? Maybe, I celebrated my 30th anniversary and my husband and I went cliff jumping into the ocean. That last jump was a bit off and I couldn’t sit for 2 days and was bruised to right buttock/outer thigh. That might have done it!?
Where is the pain? Right lower/outer buttock. Nerve pain will traverse to proximal anterior/lateral thigh, radiate down thigh over right lateral knee, then down superficial peroneal nerve (just right of tibial bone) into talus area of right foot.
Describe what the pain feels like. When sitting, driving and trying to stand up, R hip will have a throbbing pain. The radiating pain down leg is like a burning probe. At night, sometimes it will just be my lower extremity that keeps me awake.
What makes it worse? Sitting, driving, bending over with legs bent to do gardening (hip will lock up/explosive pain), doing the pigeon stretch, long days of sitting/standing.
What makes it better? Standing upright and walking, simple stretching of hip extensors, 2 Aleve am & pm.
What is your range for the Hamstring Stretch Test? Able to stretch 120 degrees and pushing ball of foot gives extra pull to hamstring and some discomfort.
What is your range for the Pencil Test? 1.5 inches
What is your range for the Touch Your Toes Test? Full ROM, green light.
Dr. Chris
Posted at 14:53h, 31 AugustHi Laura, sorry to hear about your struggle.
Sounds like there’s a lot of spaghetti being thrown at this problem.
Do they know why the peroneal portion of sciatic nerve is irritated?
– This finding does NOT explain the anterior/lateral thigh symptoms.
– The common denominator pathology here is low back, which can shoot to all of the spots you mention.
If this treatment doesn’t work, I might recommend flying to Precision Health Group in st. Louis. He has people travel there from all across the country. You may just need adhesion removed.
Jack
Posted at 21:48h, 26 SeptemberHow old are you? 56
Any trauma to the area? No
Where is the pain? About center right buttock
Describe what the pain feels like. I’ve had this problem since June 2019. I’ve been to three different physical therapy locations (one twice). Only one of the three PT locations (with the first 6 months) made some improvement due to needling while applying current into the muscle. This took me from a pain level of 9-8 to about 5-6 where I’m at now. That person left and can’t find anyone there or at other PT locations to do that to see where it leads. Currently, I’m at a pain management location where they’ve done a trigger point injection, which hasn’t helped much but only done the injection once. They say it may take multiples. As for the pain, it’s in the right buttock and feels like a knot with low to moderate pain. When sitting, the pain radiates down the hamstring, back of calf to ankle. A good bit of time, calf feels like it wants to cramp and tingling around ankle. Going from a seated position to standing pain level is around 6 with sharp pain down the leg. The pain increases until fulling standing and subsidies some what.
What makes it worse? Sitting and laying too long.
What makes it better? Standing and moving.
What is your range for the Hamstring Stretch Test? I’m in the good range based on picture. 2-3 pain level in buttock, stretching in the hamstring and feels like tingling in the calf.
What is your range for the Pencil Test? 3 in extended
What is your range for the Touch Your Toes Test? Fail/low risk can get to about 2 inches before needing to bend knees.
Dr. Chris
Posted at 15:10h, 09 OctoberSounds like a disc issue, mainly due to extension in Pencil test and laying down as a provocative.
christina yanssens
Posted at 03:42h, 09 OctoberI’ve been suffering with right buttock pain localized to the ischial tuberosity down to the back of my knee . It is worse in the car and on inclines. I have very tight hamstrings and yoga Downward dog inflame immensely. My orthopedic dr insisted it was from a slight hernia room at l2-3.. I went through 3 epidural steroid injections and now he says it’s Piriformis Symdrome. I have done PT and stretching. But no relief. I have had 3 cortisone shots that wear off quickly. I want to get back to running…anywhere to be evaluated for this in Northeast Ohio?
Dr. Chris
Posted at 15:11h, 09 OctoberSorry for your struggles Christina. The closest is likely Functional Pain Relief in Libertyville, IL. One of best chronic pain docs in country. If it’s bad enough, go there.
Debra Johnson
Posted at 16:34h, 21 NovemberHi Chris,
I am a 67 year old young lady. I have always been very active. And then almost 2 years ago, I began having pain on my right side. It has been changeable. Started in butt and around into groin and down along outside of thigh to bottom off knee. Excruciating pain on bottom of knee when trying to stand up and straighten leg. Had hip and knee xray – nothing but normal wear, had lower back mri, they said nothing that should be a problem,
s IMPRESSION:
1. Mild grade 1 spondylolisthesis of L5 on S1 without spondylolysis. Slight
increase in flexion.
2. Facet arthrosis at L4-5 and L5-S1.
3. Bilateral symmetrical sacroiliitis.
4. Possible mild compression deformities of L1 on L2 of uncertain age.
5. Calcified cholelithiasis.
Have had lots of Chiropratic and physical therapy. Still got pain, like sore knee and butt pain around into groin and plenty of trigger point on outside of thigh.
Have had hip and back injections, didn’t help for longer than a couple weeks.
I think all medical around here has given up on me. So tired of it! Getting some relief from an alleve tablet once in morning and once in evening, then at least I can walk some with less pain. Thanks
Anywhere in the Midwest where I can seek help?
Dr. Chris
Posted at 17:01h, 21 NovemberYup, sounds like low back is the problem, especially since it has wrapped to groin. Yes, we have specialists out there. Put your address in here:https://integrativediagnosis.com/find-an-id-provider/
Todd Harris
Posted at 04:13h, 25 DecemberHi, Thanks for the great site and information. Do you have a recommendation on someone in Atlanta/Georgia area who is certified to treat Piriformis Syndrome? My wife has been suffering for many months
Dr. Chris
Posted at 12:58h, 25 DecemberHi Todd, we have docs in Sarasota FL and North Carolina? Check out integrativediagnosis.com and click Find a Provider. May be worthwhile to travel.
Jon Sellers
Posted at 10:57h, 25 DecemberHi Chris,
I’m a 47 yr old male, prior to 12/01/20 I would run about 3 miles 4 times a week. On 12/01 the pavement was icy after work and I chose to walk in the grass for traction and stepped into the dirt that was mud near a fire hydrant and I sank about foot on each foot and I twisted my body trying to get out of the quick sand like feeling. The grass area was cover with frost and straw and it looked like solid ground. The fire hydrant had leaked and they repaired it and filled in dirt around it and I fell to the pavement and scraped my right knee. My symptoms are lower back pain, right hip pain with numbness, I can’t sit because it’s painful, I can’t drive because my right hip pain and numbness. I have had a MRI of my spine which indicated no bulging or herniated disc. I’m scheduled for a MRI of my Right Femur on 12/28. Do you think this is Piriformis Syndrome?
Dr. Chris
Posted at 13:00h, 25 DecemberSounds like disc issue Jon. MRIs aren’t 100% sensitive and perfect. If numbness is EXACTLY at spot we treat, it might be PS. But if I had to put money on it, I doubt it. Way more likely to be disc based on presentation. Do you have any low back stiffness or protective sensation too?
Jon Sellers
Posted at 06:29h, 28 DecemberYes I have low back stiffness and I wake up in the morning with back spasms in my lower back. I get pain relief from ice, tens unit, and laying on the floor.
Emmy Cho
Posted at 06:01h, 04 JanuaryHow old are you? 46
Any trauma to the area? No
Where is the pain? Low butt, and then down the middle of my hamstrings when I stretch
Describe what the pain feels like. Like my hamstrings are going to rip out of my butt, and I’ve been training flexibility and specifically hamstring stretching for five years and have made almost no progress (I am a dancer)
What makes it worse? hamstring stretches, esp when i try to cross my midline or internally rotate my leg
What makes it better? not stretching
What is your range for the Hamstring Stretch Test? ~80degrees but extreme pain when i try flexing my foot
What is your range for the Pencil Test? Pass
What is your range for the Touch Your Toes Test? Fail (3″ from ground)
I’m pretty sure it’s piriformis because I have had 3 bouts of sciatica, where foam rolling my butt seemed to help.
And also, I have these little rock like nodules that I can literally grab hold of deeper inside near the bottom of my butt. Also, any adhesion specialists in the DC area?
Dr. Chris
Posted at 13:24h, 04 JanuaryCould be piriformis but sounds like a disc issue. Email me at drchris@barefootrehab.com and let me know how bad it is and where you live.
Hannah K
Posted at 04:19h, 06 JanuaryHello Dr. Chris,
I am in need of your help/expertise.
Age?I am a 32 year old female.
Was there trauma? The pain started about 3 months ago for me. There was no obvious trauma that I can think of, I work an office job but I am (used to be) very active, walk 4 miles a day, workout 3 times a week, surf every other weekend.
Where does it hurt? my outer hip and deep in my gluteal area on the right side started kind of hurting one day and got progressively worse and within 3 days I was limping. What does the pain feel like?It is constant, I cannot walk without limping slightly, push on brake pedal to drive, put on pants or shoes… it’s mostly deep in my gluteal area, but radiates down the side of my thigh sometimes. What makes it worse? Bending forward too far. It hurts if I sit too long, when I lay in bed without a pillow under my knees, stairs are awful. What makes it better? standing up and being still seems to help until my left leg gets too tired, when I first wake up in the morning and I’m just laying there that helps, laying flat with a pillow under my knees. What is my hamstring test range of motion? Somewhere between 50-60 degrees. Pencil test? This was confusing, the pencil didn’t change much from when I was in neutral position to when I was arching, but there wasn’t much pencil touching my back in both positions. What is your range for the touch your toes test? About 4 inches from the ground. I’ve had an X-ray and MRI of both my hip and lumbar spine, everything looks normal, no enlargement of the piriformis, no problems with my discs. They did a round of oral steroids which really helped to quiet the pain although it was still there, while I was taking them but the pain came back full force as soon as i finished the meds. I’ve been to a chiropractor, had deep tissue massage, and seen two physical therapists, one had me stretching and strengthening the piriformis muscle, the one I’m seeing now has me doing postural therapy to correct a lateral pelvic tilt. I know you said I this blog is for people who’ve had pain for six months but it’s not improving for me very much at all. I live about 30 minutes north of Los Angeles. Do you know anyone around here who can help me? At this point I’m willing to drive across state lines or even fly out to come see you, I really need this pain to go away so I can get my life back (and hopefully not lose my job since I’ve been out for 3 months now). Thank you in advance for any suggestions.
– Hannah
Dr. Chris
Posted at 14:56h, 07 JanuaryHi Hannah so sorry to hear this. It sounds like even though MRI was clean it may be coming from low back, esp cuz of lateral hip symptoms (maybe sciatic nerrve at external rotators). Closest to you is CO. Can you fly there? That’s your best bet.
Hannah K.
Posted at 05:29h, 08 JanuaryI know it’s hard to tell just from what I’ve told you, but do you think I have an adhesion like what you described on this page? The lateral pelvic tilt isn’t confirmed, it’s just what the therapist suspects. And yes I can go to Colorado, I’m willing to go just about anywhere at this point!
Dr. Chris
Posted at 21:53h, 13 JanuaryWith a clean MRI, that means any disc pathology is likely small if it exists. Yes, your case sounds like almost every low back/butt patient we have.
See which CO provider is close to you on integrativediagnosis.com and click “find a provider”.
Elizabeth Laubenthal
Posted at 14:33h, 06 FebruaryHi Dr. Chris,
I have intermittent pain at my “sit bone”, sometimes it will grab or feel like something is hitched on the movement of standing up. This can sometimes happen when getting in and out of car. If I wait and tuck my tailbone or something like that it usually releases. Ive had about 5 times where this actually caused electricity to my groin area and maybe leg, but definitely not all the way down leg. The pain at time of electricity is 10/10. 4 times the pain last like10 seconds. But one time lasted for a period of hour and a half with initial electricity and then very tender where ai could not put weight on foot, or electricity might/would come back. I did get xrays and MRI. MRI said L5-S1 anterior spondylolisthesis, but stable., and have PT ordered. The PT thinks i have very weak gluteus medius muscle and if it doesn’t engage then the piriformis contract and hurts the sciatic nerve. So she has me doing exercises for core and glutes. It might be helping but the pain is still tender at times and if I stretch my hamstring this seems to irritate it. Do you think the PT is on the right track? Any other suggestions.
Dr. Chris
Posted at 15:00h, 06 FebruaryHi E – glue medius weakness would NOT cause “electricity” into the groin. It’s NOT physically possible. That means other nerves are compromised. My diagnostic hypohtesis is, even though it’s stable, the L5-S1 spinal segment is overloaded and stressing the lumbar nerve roots.
Core exercises may be helpful. If you can find an adhesion specialist, I’d definitely pursue that.
Elizabeth Laubenthal
Posted at 15:18h, 06 FebruaryThanks for the response. Can an adhesion specialist help with compromised nerves?
Im so glad to find this site., Thank you, Elizabeth
Dr. Chris
Posted at 18:17h, 08 FebruaryWe do all the time – like we helped John with his sciatic nerve.
https://www.youtube.com/watch?v=B3_0SzUPiyE&list=PLnKFrpVz7iNARbHRTDHp6zKPUFT2xFWc-&index=13&t=1s
Greg Sewell
Posted at 23:05h, 10 FebruaryDr. Chris,
I live in S. CA. I am hoping you can give me some help. I have been dealing with this very severe pain for the last several months. MRI showed a small disc bulge at L5/S1, so they went down that road and did and epidural injection which provide no relief at all. The pain continues. The pain is basically in my butt and then I get quite severe nerve pain down to the top outside of my foot. In the morning when I get out of be, the pain is fairly severe but I can work through it and by the time I go to work, I can walk and pain is down to about 2. But by lunch time the pain begins getting worse and steps are more painful, getting up to about 5 and progressively gets worse after that to where I often have to use crutches to walk in the evening to take some pressure off. I then got an unguided injection to the piriformis which seems to have helped slightly. They plan to do a guided injection next and I am getting PT focusing on rotating my right knee inwards to increase ROM and then also hip strength. Not sure where this goes. I haven’t been able to run or exercise for months. I just need relief from the pain. Thanks for your expertise.
Dr. Chris
Posted at 00:15h, 12 FebruaryHi Greg, so sorry to hear this. The closest adhesion docs are in CO. It sounds like you need an adhesiosn release specialist. Do you have other lifestyle contributors? How’s your diet, sleep, stress, emotional life, childhood? We may be able to help you with our 10 week virtual course, but it depends.
John Dailey
Posted at 03:35h, 03 MarchHey Dr. Chris – Im writing about my father – hes 69 years old, and last July tore his quad muscles on his right leg after missing a stair step outside his home. He had surgery to reattach, and a few months in, maybe around September, he started having pain in his right rear glute when sitting. After a prolonged bout of sitting for several days due to inflaming his quad repair, something seized up and caused severe pain in that glute. Since then he has not been able to sit for more than 15-20 minutes, and usually that is painful, and after 6 cortisone shots (1 in each hip, one in ischial bursar, one in sciatic notch, and two in piriformis he is in worse shape than when he started. He has had lumbar MRI, X-Rays, and Pelvic MRI done, all which show nothing anyone can pinpoint (I did notice something on his MRI that is maybe scar tissue that looks to be right under his nerve on the right side where his pain is,. but I dont know anyone to run it past to know for sure – Im an IT guy not a doctor so I can only go so far with something like that). My question is how do you help someone that cant sit long enough to make it anywhere to see other docs. We are located in Boone, NC and pretty desperate to find a solution for him, just the severity of his pain is such I dont know how to get him to someone other than an orthopedic here that will just want to inject him some more…I did see you recommended Dr. Shane Tipton at Wake forest which is about 1hr 45 minutes away, and Im going to call for him in the morning, and I will do the tests you mentioned when I can and post back – problem is hes in so much pain usually Im not sure I can even do the tests with him.
Dr. Chris
Posted at 15:26h, 04 MarchSorry to hear this John. There’s no really good answer. He can try oral steroids or learning how to meditate. Once people’s joints degenerate, it’s hard to get them relief. You can try performance-therapy.com, but they haven’t been doing it as long as us. Try to get him to walk for bits of rest from loading his painful spot while sitting. Drink lots of water and eeat paleo to de-inflame the body.
Gina Elliott
Posted at 12:25h, 13 MarchHi Dr Chris, I have Ehlers Danlos Hypermobility and Pirifiormis Syndrome bilaterally. Can this release be performed on someone like myself? I’m located in Virginia.
TY
Dr. Chris
Posted at 23:09h, 14 MarchHi Gina, Yes it can, we’ve helped patients with ED. On average, I’d say adhesion is causing 30-60% of the pain for these individuals. The rest is ED, muscle weakness, and often an inflammatory diet. So you’d need to find a specialist to help you with each piece. Hope that helps!
Laxmi patlolla
Posted at 12:53h, 20 MarchHi
I’m suffering with pain in my left buttocks I got X-ray and mri nothing was found. When through physical therapy. Doing stretch’s at home.
It’s been an year I’m tired of this pain, unable to sit or stand for long.
Please help
Tracy
Posted at 02:55h, 23 MarchDo you know anyone in San Diego. CA or LA that cam help with the adhesion work for piraformis syndrome?
Kseniya Conniff
Posted at 21:20h, 20 AprilHi, is there anyone in the Atlanta GA area that can help me with the adhesion? I would really appreciate any help. I’ve been in pain for almost a year.
Dr. Chris
Posted at 20:50h, 26 AprilClosest is Veracity Soft Tissue in Sarasota. If it’s bad enough, I’d travel.
Swat
Posted at 01:58h, 06 JulyHi
I read multiple comments some match’s with my symptoms.
My name is Swat and I’m suffering shooting kind of pain randomly once to multiple times in a day in my left buttock. And burning pain In my left buttock if I sit for more than 5mins. Sitting in car and sitting on soft hurts a lot. This started 18months ago with sudden sharp shoot pain (1-2 seconds 10/10 pain), it is increasing my pain level everyday . Taking stairs makes pain worst too.
I got 2 X-rays done negative 10-15 physical therapy didn’t help went to 10 chiro sessions, chiro told my neck is bend on X-ray it looks like military neck. Chiro gave treatment which also did help me. I took a break and went to née pt he did elbow massage my sharp pain didn’t come back in 4weeks but after stopping that I got same issue when I took 3 hrs flight. Continuous sitting is hurting me. The pain iss only left buttock I don’t know if it sciatic or piriformis issue. I met 2 doctors 2 X-rays 1 mri 18 pt sessions 10 chiro
Please help I need expects helps can’t bare this pain
I’m 30yrs I don’t want to go through steroids or sugary as I want to plan for kids
Dr. Chris
Posted at 12:48h, 06 JulySo sorry to hear this, what did the MRI of low back say?
What is your Pencil Test Measurement?
Adewale Adeyemi
Posted at 11:31h, 11 JulyHi Dr. Chris. I have been having piriformis syndrome for more than 6months. I started experiencing it after I took typhoid injection.
Please which of your treatment should I use
Dr. Chris
Posted at 13:19h, 05 AugustHard to say. I’d try a strict 30-60 paleo diet as recommended by Chris Kresser as the typhoid injectino implies that you have gut dysbiosis.
Then, you should look into an adhesion doctor or therapist.
Thomas Lewis
Posted at 23:41h, 12 JulyDr. Chris,
After chiropractic care, pt, hip injection, back injection, aqua workouts. Sacrowedgy, foam roller., Motrin, Aleve, Blue Emu, CBD lotion, menthol gel, ice, heat…over the past 6 months, still suffering from piriformis pain (sciatica, hip, back of leg, It band, knee, & top of foot).
OK, playing golf 4-5 days per week might not be helping my condition. But I did make my first hole in one back in March & just can’t stop now!
Any suggestions for a PS specialist in Grand Rapids, MI?
Dr. Chris
Posted at 13:20h, 05 AugustGo see Dr. Eric Lambert at Discover Soft Tissue. He does adhesion work. You haven’t had this done yet and this helps most people in chronic pain.
Sara
Posted at 23:50h, 12 AugustHi Chris. I have pain in lower back pain in left hip pain left glute pinching in hamstring pins and needles in foot . Any idea what this is maybe sciatica
Dr. Chris
Posted at 00:02h, 13 AugustHi Sara, it sounds like a disc with radiculopathy. It hits all your points. I’d get an MRI and get the disc treated by an adhesion specialist.
Stephanie Schmoyer
Posted at 02:58h, 18 AugustHi Chris!
I’ve read through many comments above.. I have similar experience. I was experiencing butt pain in the last pregnancy. Two weeks postpartum, I stood up and pain radiates from the butt to the ankle. After many chiro adjustments and glute strength, I’ve centralized it to mainly the left butt. I’ve tried a lot of PT, injections at L4, L5 and two in SI joint. Pain when rolling over, pain after waking up and standing for 20 min, I become hunched. If I sit for 20 min, I can’t stand up straight. The pain is in the upper center butt. I feel tightness in the back of the thigh. I’ve tried release therapy, massage, chiro, PT. Dry needling. Most things irritate it more. I’ve Been in pain everyday for 16 months.
I have a “slight” hernia at L4, Drs didn’t seem to think it would cause this amount of pain.. the L4 injection helped for 3 days and then the pain came back.
It seems like PF, I have a lot of pain raising my left leg up off the ground.
I’m in Cincinnati oh.
Thank you!!
Stephanie Schmoyer
Posted at 03:03h, 18 AugustAlso, I saw a comment about “cat cow”. I just told a PT that I can stretch through Cat and the when I push the butt up for cow, instant sharp pain.
Dr. Chris
Posted at 15:48h, 19 AugustHi Stephanie, the “cow” confirms that your disc is referring pain. We have a couple adhesion docs in OH. GO here –> https://integrativediagnosis.com/find-an-id-provider/
I wouldn’t bother with regular therapy. If you have adhesion you need it removed.
Sara
Posted at 12:52h, 20 AugustHi Dr Chris. I have pain in lower back pain in left hip pain left glute pinching in hamstring pins and needles in foot . Any idea what this is maybe sciatica
Thank you for getting back to me. I did have an Mri and they said I have a bulging disc but not leaning on any nerves and I have wear and tear. Is it still possible to have this with a bulging disc with no compression. Thank you
Allison Hendricks-Smith
Posted at 17:29h, 06 SeptemberThis is the first article I have read, in a year of struggling, that describes my symptoms to a tee! Can you advise the closest specialist to Albuquerque, NM? Thank you!
Dr. Chris
Posted at 21:16h, 08 SeptemberHi my friend, glad to help. I believe closest is CO or St. Louiis. Check it out here: https://integrativediagnosis.com/find-an-id-provider/
Madison
Posted at 01:34h, 28 SeptemberHi Chris,
I am a 26 year old female. I believe i Injured myself 5 months ago using an abductor machine at the gym. Simce then i have had pain in right buttocks and hip that moves down the leg sometimes into my knee when inflammed. It doesnt matter what exercises or stretching i do the pain continues to come back. Your article explained what i am experiencing and i was wondering if you know of any providers who live in Bali? Thanks so much
Dr. Chris
Posted at 18:56h, 28 SeptemberHi Madison, sorry to hear about your pain. Hmmm, your best bet is to find a rolfer or a really good myofascial therapist. There aren’t many of us adhesion docs in the world, but you never know, you might find someone who is good. Let us know how we can support.
Kevin
Posted at 17:05h, 18 OctoberHello Chris – can you recommend someone in the Birmingham, AL area? I’ve had very significant glute/hamstring pain for 4 1/2 years now. Occurs when sitting. It started during a long car drive a couple of days after a fairly intense HIIT session on a treadmill. I had a bit of a layoff and jumped right back into HIIT. That may or may not be relevant. P.S. was ruled out after provocative testing. I’ve had a ton of diagnostic ESI’s in an effort to attempt to identify the pain generator. ESI’s to date: piriformis muscle; sacroilliac joint; ischeal bursa; L4-L5; L5-S1; cluneal nerves (all 3); and – last week – the hamstring tendons tie-in spot on the sits bone, which gave me significant relief as far as the back of my leg, but none at all as to the glute. It’s pretty awful. Thanks man, K.B.
Dr. Chris
Posted at 17:24h, 19 OctoberHi Kevin, closest to you is probably a Precision Health Group in St Louiis. If it’s bad enough, I recommend you fly there. He’s one of the best docs in country. No one is closer.
Kristin
Posted at 20:22h, 27 DecemberHi there, Are there any providers that you know of in the Boston area? Thank you!
Dr. Chris
Posted at 21:29h, 27 DecemberHi Kristin, look up Dr. Keith Puri. He’s a colleague of mine. Full disclosure, I don’t know how much he’s been doing ongoing training, but he at least knows this system. I also don’t think he has the soundwave technology we use to break up adhesion. We may be the closest. Up to you.
Nigel McKAY
Posted at 22:38h, 06 JanuaryChis I live in Panama City Beach Florida is there anyone in Florida, Alabama, or Georgia that has similar training that I could see, I am a retired DC who through my repetitive stresses from manipulating so many patients in a high volume practice. I’ve had left butt pain since 2010. I have been through the mill and spent thousands of dollars and many fruitless hours in many clinics, Chiros, PT’s, Acupuncture, laser disc surgery, steroid injections, opiate drugs and even a $3000 stem cell injections.
Dr. Chris
Posted at 19:46h, 10 JanuaryHello my friend – TY for the work you did. Only one certified Adhesion Release doc in FL –> https://www.veracitysts.com/
Glen
Posted at 14:42h, 02 FebruaryHave you seen piriformis syndrome present as bilateral foot pins and needles, almost exclusively? No butt pain and very rare leg pains. Everything seems to trigger it other than laying flat. Pretty much everything else is ruled out.
Dr. Chris
Posted at 18:12h, 13 FebruaryIt’s possible, but it’s WAY MORE LIKELY to be a midline Disc problem or stenosis problem in low back. I’d foocus there. It all depends on your exam. If youo’d like to do a virtual consult with one of our docs, just email us and we can make that happen.
Jeanne Hergenrother
Posted at 00:14h, 13 FebruaryHi Chris,
Thank you for this information. I’ve been experiencing pain for over 6 months now, despite trying ice and heat, yoga, massage, chiropractic sessions, stretching, strengthening, NSAIDS, naturopathic herbs and minerals, etc. It started when I sat in a moving truck traveling across the country for 11 days (towing goats). Based on your description, it’s very possible I have adhesions in one or more of the muscles affecting my sciatic nerve. I’ve answered your questions below:
I’m located in Midcoast Maine (Thomaston). Can you recommend anyone in New England, or preferably, coastal Maine who could try the manual release techniques you describe? I looked on the IntegrativeDiagnosis website and see there is someone on Fall River, MA. Are you familiar with them and is there anyone closer to me?
Here are my answers to your questions:
How old are you? 61, very active (avid hiker, trail runner, xcountry skier, daily dairy goat chores and goat walks)
Any trauma to the area? Not that I recall
Where is the pain? Starts in the right butt, sometimes have dull, achy pain going down back/lateral side of upper leg into calf.
Describe what the pain feels like. Sometimes in the butt it is a tight clenching feeling. Down the leg it feels like a mild to strong dull achy pain. Sometimes some tingling down into the foot.
What makes it worse? Standing still.
What makes it better? Usually brisk walking or going for a hike. Sitting, laying down. Sometimes sitting on a hard chair is uncomfortable.
What is your range for the Hamstring Stretch Test? Over 90 degrees – probably around 110. I’ve been doing a lot of yoga and stretching in an effort to heal what I think is Deep Gluteal or Piriformis Syndrome. The hamstring stretch tended to reproduce the butt pain mildly, and pushing down on ball of foot increased the pain slightly. It actually felt somewhat good to have my husband stretch my leg like that.
What is your range for the Pencil Test? Flat for about 2.5″, so 80% lower back function.
What is your range for the Touch Your Toes Test? Backs of all fingers flat on floor easily, stretch felt in hamstrings, not calves.
Thank you!
Dr. Chris
Posted at 18:15h, 13 FebruaryHi Jeanne! So sorry for your length of pain. Dr. Dersham are really good doctors, it would be worth a try. Not sure how confident they are based on the chronicity of your pain. It sounds like a disc problem, not PS. If they can’t help you, you may need to fly down to see us. We have patients fly in from across the country (if it’ bad enough). Here for you.
Darlene Milito
Posted at 21:38h, 18 FebruaryHello Dr Chris its almost impossible to find a doctor who can diagnose my piriformis problem. Recently had mis l5 decompression which didn’t help a bit. Please advise if you can recommend a doctor in the Chicago area. Thank you!
Dr. Chris
Posted at 12:29h, 01 JuneHi Darlene, you’re in luck. Checkout Functional Sport and Spine in Libertyville, IL. ONe of best in country. Dr. Carl Nottoli.
John Hall
Posted at 18:23h, 31 MayHello Dr. Chirs,
I am trying to find someone in the Houston area that can do the adhesion therapy. It isn’t a herniated disk, All the tests are negative, It is an elongated Piriformis muscle. So stretching does no good. I used Ice for a while and it helped. I can feel tightness in my buttocks. And it is tinder to the touch on the buttocks. I have pain in the buttocks and shooting down the back of the leg. Sometimes I get a “catch” in behind my knee. Hard to explain, not a painful situation, just a loss of control. It is somewhat painful but not as much as my buttocks. The tingling/pain radiates down the side of my calf and into my foot. The Achilles is painful just on the right side. And is painful when the buttocks are involved. I feel tightness in the buttocks when I lay down on my side. Ice lately helps while I am still, on my side. It is quite painful once I get up to walk, and takes a while to work it out. As the day goes on, I am able to loosen up and move better. I still have a dull pain at all times. Any practitioners in the Houston Area?
Dr. Chris
Posted at 12:28h, 01 JuneHey John, we dno’t have provider in Texas. Closest to you if the pain is bad enough is Precision Health Group in St Louis.
Chris
Posted at 16:00h, 29 JuneAny recommendations for someone to see in Oakland County MI?
Dr. Chris
Posted at 17:18h, 30 JuneDiscover Soft Tissue Dr Eric Lamberts office is the only adhesion doc in MI!
ian m
Posted at 22:33h, 12 JulyAny recommendations for people to see in Boston?
Dr. Chris
Posted at 22:54h, 20 JulyDr. Keith Puri is your best bet.
Carolyn Laird
Posted at 18:24h, 28 JulyHi,
Is there a doctor to see in the Ogden, Utah area for the non-surgical method for piriformis syndrome? I have been doing physical therapy for 3 months. Thanks for the hope!
Carolyn
Dr. Chris
Posted at 22:41h, 29 JulyI believe closest is Precision Health Group in St Louis. They have people fly in from across the country there.
Andrea B
Posted at 08:16h, 15 AugustHi, I’ve been diagnosed with Piriformis syndrome. Physical therapy nor injection gave me relief. Is there a doctor you recommend near Hattiesburg, Mississippi?
Dr. Chris
Posted at 17:18h, 15 AugustHi Andrea! The closest is Precision Health Group in St Louis!
Jamie Cannady
Posted at 10:43h, 25 SeptemberI have been begging doctors to help me figure out my pain. This sounds like it and I have been suffering for 3 years in pain. Only being told what it is not (not a disk) but no answers or relief. I’ve done most of the treatments you listed. Pain management injections, PT, stretching, muscle relaxers, anti inflammatory meds etc. Can you list doctor in NC? Is it Dr. Tipton mentioned in article that I need to see? I want to find a doctor to help me chase down the cause of pain. I’m ready for relief and sleep after years of pain and no answers.
Dr. Chris
Posted at 18:24h, 28 SeptemberYou’re in luck. There’s an adhesion doc there, very good guy.
https://www.performance-therapy.com/
Dr. Chris
Posted at 14:40h, 23 OctoberHi Jamie, Performance Therapy – Mike Danenberg – he’s your best bet to diagnose you correctly.
Hannah Hemry
Posted at 15:39h, 30 SeptemberHi Chris!
Thanks for all the helpful information. I’ve been suffering from from buttocks pain for about 2 weeks. I’m a runner (nothing intense) but it’s killing me to not do my daily workouts and just wanting to get some relief. Right butt cheek pain is deep and walking and running makes it worse, standing better than sitting. At first hurt to walk but not better. Stretching feels fine and it’s less painful if I stretch twice a day. However it’s still very present and I can’t bend over well or even put on pants which are kind of essential when you have two little kids to clean up after. Worse towards end of day. I need to fix this! Do you have any recommendations in the portland oregon metro area? Or elsewhere in the Pacific Northwest? Do doctors perform these adhesion therapies or physical therapists? Can a chiropractor help? Thanks in advance.
Dr. Chris
Posted at 21:02h, 03 OctoberHi Hannah! So sorry to hear this. It’s probably a disc problem. Can also be a sciatic nerve entrapment. I wish we had providers there, we don’t. We are trying to train adhesion docs as we speak. The closest to you is probably Colorado – Avail Soft Tissue. You can always try a myofascial therapist who is good if you can find one.
John Baranco
Posted at 18:01h, 10 OctoberHey Dr Chris! So I had an injury from deadlifting in my low back that I thought might have been disc related but after almost 3 years of no relief and tons of cramping and pain in my piriformis (including an X-ray that shows very normal disc health for a 35 year old – how old I am) I just can’t find anything else it could be. Stretching has not helped and I also stay healthy by doing the Peleton bike and body weight exercises but it’s gotten so bad I can do normal life. It’s mainly in piriformis and cramps when I lie down for a long time or sit. Exercise takes away the cramping but it come right back when I rest or take a break. Picking up something or reaching out in front of me can cause cramping as well. I also can’t run or play golf anymore due to extremely weak feeling where the piriformis connects in the low back or sacrum. Feels so weak when I jump at all. I’ve done PT and also stretching routines but not helping at all. I’m at my wits end. I also played golf collegiately and was in law enforcement where I was in jiu jitsu and power lifting. X-ray came back with everything looking normal and even got tested for degenerative disc disease which I tested negative for. The only relief I get is when I take heavy anti inflammatory drugs and muscle relaxers but I do not take them for health reasons and not wanting to get addicted to muscle relaxers.
Dr. Chris
Posted at 14:38h, 23 OctoberSorry to hear all of this John . Just because your images are clean doesn’t mean it’s not a disc issue. The “Lying down” provocative factor makes me think disc. You’re young enough and fit enough to exercise and take stress off the disc but then it comes back. Can you find an adhesion release provider?
Courtney
Posted at 15:04h, 17 OctoberHey there!
I’ve been struggling with butt and leg pain for years now. Constant pain 24/7. Going to PT to help. All of the imaging is clear. Any recommendations if this is actually pirformis syndrome? If so, does it take a while to heal if I’ve been having it for so long?
Thanks!
Courtney
Dr. Chris
Posted at 14:36h, 23 OctoberPiriformis syndome is NOT usually constant. It’s way more likely that a disc problem is constant. MRIs are only about 70% sensitive so they don’t pick up all problems. Get another MRI and try another radiologist so you can find what’s actually going on with the low back.
Andrew OReilly
Posted at 12:14h, 24 OctoberAnybody closer to Philadelphia or just northern NJ?
Dr. Chris
Posted at 16:20h, 02 NovemberHi Andrew, we are the closest. We have many patients from PHilly, west of Philly, Maryland, and Delaware.
John Caple
Posted at 04:26h, 10 NovemberHi Dr Chris! Can you recommend someone in the Denver area? Thank you.
Dr. Chris
Posted at 20:44h, 23 NovemberHi John!
Yup Avail Soft Tissue Dr Holen or Apollo Soft Tissue – both are adhesion clinincs.
John R. Hughes
Posted at 16:58h, 15 NovemberHi Doc,
Seeking referral in California for treatment of adhesions causing my PS. Your guidance please.
Thanks!
Dr. Chris
Posted at 20:44h, 23 NovemberCoast Soft Tissue Dr Mike McAlister is the only one in CA.
John Caple
Posted at 19:29h, 26 NovemberThank you Dr. Chris. I really appreciate your help!
John Caple
Dr. Chris
Posted at 20:38h, 27 NovemberAnytime John.
Mindy Leveille
Posted at 04:57h, 27 DecemberI am in so much pain due to this, when anyone even touches the muscle I scream. The pain is a 1000! Over 3 years of a dead left leg, numbness and tingling down the entire leg like it’s asleep 24/7. Pain now is unbearable, and truly makes me question life at this point. Was diagnosed by my Physiotherapist, but nothing has helped, and my pain and symptoms have just become worse.
Physiotherapy 3x per week for over a year
Chiropractor
Botox
Steroids
Nerve Blocks
Acupuncture
Pain Doctor x2 years
Nothing has worked. Diagnosis is Bursitis, Arthritis(osteo, rheum, psoriatic), and Piriformis Syndrome. Also diagnosed in 2003 with Small Fibre Neuropathy. Bowel and Bladder/Kidney/Urethra issues
I’m 41, live in Canada, fractured tailbone x4 at a young age. Danced professionally. Have disc issues, but told not the issue. Extremely flexible(not my left leg any longer), and could bench 540 lbs consistently with legs!
Feel surgery is the only option!? I am overweight now due to prednisone, but have recently lost 50 lbs, and continue to lose!
I do live a 2 minute drive to Western, New York.
Dr. Chris
Posted at 14:02h, 27 DecemberHi Mindy,
I’m so sorry for what you’ve been through. We see this all of the time.
How bad is your MRI? I’m really curious about the lumbar MRI. It looks like your lumbar disc is really bad. The small fiber neuropathy is interesting, but doesn’t explain your symptoms. A really bad disc issue does.
Surgery might be the only option, but you need a good diagnosis, exam, to figure out details first. If you can make it to New Jersey or to Buffalo area, one of our adhesion specialist docs would be really valuable for you.
AJ C.
Posted at 03:52h, 18 JanuaryHello, I have watched your YouTube videos and came across this post, love the details. I was wondering if you had any recommendations on getting adhesion release from a doctor here in Hawaii? I am highly interested in cornering this.
Dr. Chris
Posted at 15:49h, 18 JanuaryHi AJ, I have a massage therapist who will be starting to train with us next Wednesday. Nate Ho. Stay tuned, Hoping he will be ready in 2 months.
AJ
Posted at 19:16h, 26 JanuaryThank you so much for the update! I’m looking forward to this, please let me know when he will be ready
Dr. Chris
Posted at 14:42h, 14 FebruaryFollow us on social media and we will let everyone know there! Or just reach out in a few months.
Tesfu Engida Teshome
Posted at 18:41h, 11 FebruaryHi Doctor, I am Tesfu Engida from Ethiopia suffering from piriform syndrome for the last 5years, and it gets worse at night while in bed and the mornings, need to massage for 1 hour to get relief, there is no permanent cure, will be very happy if you help me get rid of this pain from the right buttock, back middle of the thigh, back middle of the calf, One more point to add I had MRI a while ago and it came with the result likely suggests a small meningioma ddx includes small schwannoma. my email id is tes3869@gmail.com.I am from
Will be very happy if you help guide me to relieve this severe pain.
Dr. Chris
Posted at 14:41h, 14 FebruaryHi Tesfu, your problem sounds spinal. I can’t help you without seeing you in the office, which is how we help people. You need to get the spine treated. Most helpful would be adhesion release.
Terri
Posted at 22:03h, 15 FebruaryHi Dr Chris,
I live in AZ and wonder if you know of somewhere here I can go, I have done all kinds of PT, injections and chiropractic care. Watching your videos gave me hope that I could try this type of therapy.
Dr. Chris
Posted at 20:27h, 16 FebruaryHi Terri, there are no adhesion specialists in AZ. There are in CO and we are training one in Nevada but he won’t be ready for a few months. Can you fly? St Louis Precision Health Group is the best in the country.
Tabitha
Posted at 08:28h, 26 FebruaryThe method of checking the angle of the spine by yourself is very helpful
Dr. Chris
Posted at 22:41h, 26 Februaryso happy to hear!
Paul Campbell
Posted at 02:54h, 09 MarchDr. Chriss
I first want to thank you for reading and answering all these posts. That
says good things about your character. To get to the point I have pain deep in my glute that follows the path of the piriformis muscle..
it feels like the left side muscle is much larger and harder than the right. I don’t have shooting nerve pain. I’vee had it for years and it’s activated by sitting and walking. It’s especially bothered by any one leg exercises like lunges. I have an l5 s1 bulge confirmed by MRI but I don’t think that’s causing my pain as I had periodic back before the piriformis started since I was young. When my back acts up it is a different kind of pain. The piriformis pain is more predictable like the muscle is just enlarged and tender. I’m healthy, young, and have seen lots of pts with no cure. I live in little Rock Arkansas and would rather not travel far if possible as it’s hard for me to sit but I’ll do anything to get better. I would love to find someone local to try to remove the adhesion. I’m also considering a diagnostic shot in my lumbar to rule out the disc. Can you recommend someone near by or tell me what type of doctor or pt to look for to help me out? Thanks a million in advance. Been struggling with this for years.
Paul Campbell
Posted at 13:06h, 09 MarchOh and pencil test shoes healthy back.
I’m 39
No trauma
Hamstring stretch is good
And I’m green light on my stretch.
My piriformis side hamstring is tighter than the other side though.
-Paul
Dr. Chris
Posted at 14:32h, 09 MarchIt’s hard to say without doing a full history and exam. But it still sounds like a disc problem. The honest thing about low back issues is that they change and get worse as we get older when they aren’t fixed. Just because you’ve had a disc symptom that felt a certain way doesn’t mean it won’t change how it presents.
THere are no adhesion specialists in AK right now. Closest is MO? We are working on training chiros, MTs, or PTs if you know anyone who want to learn this in your area.
J Kaus
Posted at 18:57h, 06 AprilI am in Kansas and am looking for your recommended piriformis adhesion specialist nearby (KS, MO, NE, OK). Thanks!
Dr. Chris
Posted at 12:28h, 07 AprilHi there, our teachers and the best in the country are at Precision Health Group outside of St Louis, MO. I would go straight there. They have people flying in from across the country.
courtney
Posted at 23:39h, 06 Aprilhi dr chris!
i have been having deep glute pain for 5 years now which calf sciatic pain and aching. i have been diagnosed with IFI and quadratus femoris edema. Not sure where my sciatic nerve is stuck but it is for sure stuck somewhere. my lumbar MRI is clean along with my EMG of lower extremity. the pain is constant. do you think this is more of a pirformis issue or sciatic nerve entrapment elsewhere?
Dr. Chris
Posted at 12:30h, 07 AprilIf the pain is constant, it’s mostly likely a lumbar disc issue, even with a clean MRI. Remember, MRI’s aren’t 100% perfect technology. The reason why is most people can take enough stress off of a sciatic nerve entrapment at glute, ham, or calf by laying down and having no pain. But your pain is constant, suggestsing that a disc is damaged. Yes, the QF edema is an issue, the question is, what’s the biggest priority to get you the fastest and most permanent relief. Hope this makes sense to you.
Allison McCann
Posted at 19:55h, 23 JuneHi,
I am a 25 year old woman and I have been diagnosed with piriformis syndrome. I have had pain (glute ache, tingling in foot) for the past 2 years without any lasting improvements. I did not have trauma to the area. It came on when I was training for a half marathon and sitting for long periods of time at a desk job. It came on about a year after I graduated college, where I I was D1 college tennis player. I lost a lot of muscle when I stopped playing tennis after college. I have had 3 MRIs (lumbar spine, sacrum, pelvis) and all have been completely normal.
For treatment, I’ve seen multiple doctors and have done extensive PT, massage therapy, dry needling, yoga, stretching, rest, and had a steroid injection in my piriformis. My pain started as an ache in my glute and down my hamstring for the first year. I was doing PT and was still relatively active without terrible pain. I continued to do PT and then started getting a tingling in my foot about 8 months ago (it varies where I feel it in my foot. I don’t feel any tingling in my leg). Since then, I continue to have the ache in my glute, tingling in my foot, and ache/tightness down my hamstring.
It is very up and down. Standing and sitting for long periods of time make it worse. My pain is rarely greater than a 4 or 5 on a scale of 1-10. I would describe it more as discomfort most days, with occasional bad flare ups. Rest doesn’t necessarily make it feel better, although I have completely stopped running. Ice and medicine don’t help much.
1. What is your range for the Hamstring Stretch Test?
—Bad range. Feel a stretch but it does not reproduce pain.
2. What is your range for the Pencil Test?
— Flat against low back for 1.5-2.0″, then rounds off.
1. What is your range for the Touch Your Toes Test?
—I fail this test. I am not close to my toes, but I have been super inflexible my whole life. I can’t remember ever being able to touch my toes.
Dr. Chris
Posted at 20:31h, 23 JuneSounds like a disc problem with a sciatic nerve entrapment. Where do you live? You need to see an Adhesion Release Methods provider.
Gloria Kain
Posted at 12:03h, 25 JuneWhere is there an Adhesion Release Methods Provider in the eastern Massachusetts area?
Dr. Chris
Posted at 12:33h, 26 JuneYou’re in luck, there’s ONE. Dr. Todd and stacey Dersham. Health Source All River. Let us know how it goes if you see them.
Chelsea
Posted at 00:24h, 23 JulyHi,
I’ve been dealing with peroneal nerve pain in my calf and sciatic nerve pain in my hamstring. I’ve been on the active release website to find a nerve entrapment specialist around Cambridge,MA. I’ve seen three specialist who have tried to help but don’t seem to know what they’re doing especially when it come to releasing the peroneal nerve. I’ve looked everywhere and the only thing I’ve found is this video but they’re in Canada
https://www.youtube.com/watch?v=Gpnpe0hik2g&pp=ygUncGVyb25lYWwgbmVydmUgcmVsZWFzZSBwaHlzaWNhbCB0aGVyYXB5
Im at a breaking point where I’m willing to go to Canada to get the right kind of help.
Is there anyone you know who can help in the US or is this something that you can help with?
Dr. Chris
Posted at 14:10h, 23 JulyHi Chelsea, so sorry to hear this. We help this all of the time. Dr. Chris saw 4 patients last week with sciatica and peroneal nerve pain.
Chuck Crisco
Posted at 02:19h, 18 DecemberMy apologies, as I know you get bombarded with requests for information about providers that are closer than you are. I tried to use the integrative site you mentioned above but it is no longer active. I am in Florida and looking for something a bit closer. Can you please recommend? I’ve watched a bunch of your videos and I think the adhesion approach may be the answer I have been looking for, for a long time. Help?
Dr. Chris
Posted at 21:37h, 20 DecemberHey Chuck, there’s only one in Florida. Veracity Soft Tissue Dr Andy Wengert
James Prizzi
Posted at 17:00h, 30 JuneHello Doctor,
I have been suffering for about a month now. The burning sensation on my but is constant. My legs are very sensitive to the feel of the fabric of my pants (soft cotton) and I tried the exercises that were recommended on line. I think the exercises made it worse. Sitting is torture and I can’t find a doctor that specializes in Periformis syndrome and I live in New York City where you would expect to find the best of the best.
I have not injured my back so I don’t understand where this came from. I do work at a desk 8 hours a day five days a week and I am 74 years old.
Help!
James
Dr. Chris
Posted at 16:47h, 15 JulyHi James, I’m so sorry to hear this. Dr. Mike V at Wildcard Spine and SPort is one of our instructors for Adhesion Release Methods. I recommend you go see him.