
21 Dec Got Hip Bursitis? Beware of Short Term Relief
Hi Dr. Chris, I have hip bursitis. What should I do to stop the inflammation?
Dear (name),
So, you have hip bursitis?
And you want to get better, quickly, and for good? Without the possibility of relapse?
I’m so happy you emailed.
Now, about your question, “What should I do to stop the inflammation?”
My question back is “Is that really all you want to do, stop the inflammation (and get short term relief only)?”
If you’re stuck on that question, then you have options. Conventional physical therapy, chiropractors, and orthopedic doctors are armed with tools to de-inflame you: ultrasound, electronic stim, ice, heat, massage, manual therapy, foam rollers, cortisone, etc.
That stuff’s great and necessary. But if you stop with that question along, you’ll only get out of pain in the short-term.
If you want to get out of pain and prevent pain in the long-term and stay as healthy and fit as you want into old age, keep reading.
What is hip bursitis?
Every time a patients walk into our office with the diagnosis “hip bursitis,” I throw up a little in my mouth. Without any more information behind the diagnosis, the pain is destined to come back due to the wrong treatment for the wrong problem.
Kind of like using a hammer on a screw.
The first reason for my disgust is there is often no inflammation. The “-itis” part of the diagnosis indicates inflammation. The hallmark signs of inflammation are redness, swelling, heat, or pain. If bad enough, you can feel liquid under the skin. In reality, there is usually no visual or palpable evidence of redness, swelling, increased temperature. There is only pain.
Pain, alone, at the hip, is not good enough to be labelled “hip bursitis.” Many hip conditions have pain. If you walk in with an MRI that shows inflammation in the bursa, then I’ll eat my words because you really do have hip bursitis. This is often not the case for people diagnosed with hip bursitis.
The major, second reason for my disgust, is that “hip bursitis” tells you nothing major as far as why you have hip pain.
When the term “hip bursitis” is used, the location is typically right above the widest, most outside part of your hip.
Symptoms at the widest location may be called “trochanteric bursitis.”
Bursitis is when the bursa is inflamed from too much stress, usually from the IT band and its associated muscles pulling extra tight, pushing the bursa excessively into the bone.
I agree that the pain generator, or the tissue that is damaged and pissed off, can be the bursa.
But the pain generator is more commonly not the cause of the problem.
Treating the cause of the problem is key to permanent hip pain-free living. Otherwise, you could become a victim to the Kitchen Sink Paradox. When your pain isn’t getting better after 10, 20, or 30 treatments, or after several months of care, you’re in trouble.
Key Take-Home Point #1: If all you’re doing is de-inflaming and getting treatment for the pain, you’re missing the boat.
The Truth Behind Hip Bursitis
The question you should be asking is:
Dr. Chris, I have hip bursitis. How do I get out of pain now and make sure that I never have a hip problem for the rest of my life? Remember, I plan on living to 100!
As a life philosophy, when your muscles are flexible and strong, you can do what you want to do and have little worry about pain.
When muscles tighten and you start to get weak, the rabbit hole to figuring out why you have hip bursitis pain can be very deep.
If you have hip bursitis, it’s safe to assume that your IT Band is being asked to do too much work. Working overtime is never fun, even for our muscles. And any muscle that is compensating for another muscle will scream out in pain, at some point.
Why is the IT Band doing too much?
The IT Band is a secondary knee stabilizer when the hamstrings, your primary knee stabilizer, are not functioning at 100%.
To have a fully functionally hip and posterior chain (including the hamstrings), you need to have flexibility in the following tests (you can test all of them in 10 minutes with a friend, a ruler, and an observant eye):
- 90 degrees (thigh perpendicular to the ground) in your hamstring stretch test.
- Your thigh touches your chest in the thigh to chest test.
- 12″ in the lunge stretch test.
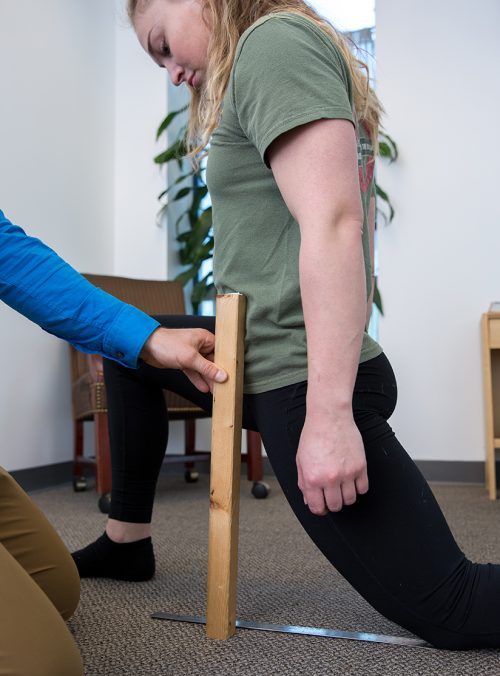
All you need to measure the lunge stretch test is a ruler and a straight edge to pinpoint where the front of the hip is over the ruler.
If you don’t have full range of motion in any of those tests, the hip joint and the associated muscles are compromised. When one muscle works at 50% function, another muscle has to go from working a normal 100% capacity to 150% overtime to compensate.
In the below image, notice the ankle has been overloaded (the red spill out of the bucket) and is now working at 90% capacity. That means the hips have to compensate and work at 110% capacity.
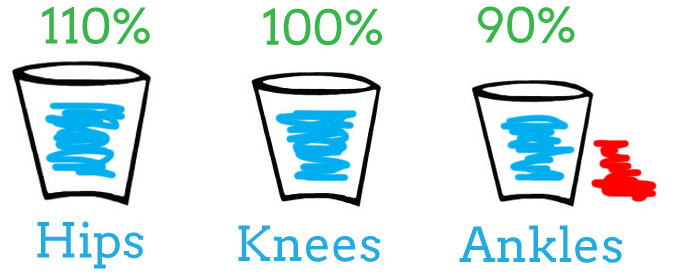
Now, if your hamstring stretch test is 90 degrees, but your knee caves in when you lunge, your hamstrings are weak and your IT Band is compensating. In the video, the caption cites a sciatic nerve entrapment. The caption is only correct if your range of motion is less than 90 degrees.
If you have true hamstring weakness, any hamstring strengthening exercises will help.
What Should You Do Now?
The function of your joints matters enormously.
The three-step process to getting out of hip bursitis pain for good is:
- De-Inflame (according to traditional hip bursitis protocols)
- Restore your joint range of motion and function in all relevant lower body tests (the most ignored part of getting healthy and pain-free).
- Progressively increase load of all lower body and core muscles (what physical therapy exercises attempt to do).
Because #1 and #3 are common practice, I’ll speak about #2 quickly.
You can attempt to stretch and gently do dynamic exercises (air squats, cossack stretch, lunges) for a month to see if you can increase your range of motion. If your range increases, wash, rinse, repeat, and keep doing what you’re doing. If your range of motion doesn’t improve at all, stop doing it and find out why by getting a diagnosis and undergoing manual therapy. Integrative Diagnosis (ID) providers are the most skilled musculoskeletal practitioners at diagnosing problems and restoring range of motion.

Some strength coaches, chiropractors, physical therapists, and massage therapists can help too. But the percentage of competent professionals in those categories is much smaller compared with ID providers.
Remember, the question frames your behavior and can be the difference between a lifetime of pain-free living and a quickly degenerating joint when you ignore the reason for the hip bursitis in the first place. While conventional de-inflaming is necessary, it’s only the start to getting healthy again.
Proceed smartly.
If you live in New York City or Northern New Jersey and you want a humble opinion about your pain and what caused it, please come see us at Barefoot Rehab. We know how to set you up for long-term success.
Love always, Dr. Chris


Barb Dinges
Posted at 06:45h, 12 JanuaryI had a broken hip and thigh they put in a l and screws now I havef it and bursitis at the end or top of the appliance. What do I do it hurts rts and I can,t move that to leg up or step on it………..
Dr. Chris
Posted at 01:05h, 13 JanuaryHi Barb,
All of Teri’s thoughts are worth giving a shot. Besides that, having a specialist check for adhesion and slowly strengthening with physical therapy can be helpful too. Let us know how it goes?
Barb Dinges
Posted at 06:47h, 12 JanuaryPut in a. Nail….
Teri Hill
Posted at 08:46h, 12 JanuarySee my reply below. I accidentally made a new post lol. I was tired.
Teri Hill
Posted at 08:45h, 12 JanuaryI have had chronic bursitis in both hips for close to 5 years now. I’m so sorry to hear that you are suffering this pain too. I’m going to tell you to use cold compresses on it to help with the inflamation right now. Trying to keep the joint as immobilized as possible is helpful too.
When you go to bed, be sure that you are sleeping ONLY on your back! It might take you some time to get used to doing this, but let me tell you what, it will help you SO MUCH with your bursitis pain down the road, i promise you! If you lay on either hip, you are going to pay DEARLY, waking up screaming your head off feeling that flaming torch feeling because you are going to cause that iliotibial band to stretch across that swollen bursa sack. You want to be sure to be on a soft mattress with your knees bent slightly outward and your feet kind of pulled in toward the center like if you were going to touch your heels together. I had to purchase a 3 inch gel mattress pad to place over my mattress because even my medium mattress turned out to cause me major issues. I also sleep slightly elevated.
Something else that helps is Epsom Salts diluted in warm water, and soak a wash cloth in it. Lightly wring it out and blot it on and hold it onto the skin over the pain for a few minutes, or rub it onto it…as long as you don’t have any stitches in that area of course. Magnesium, which is what epsom salts is made out of, is a major, natural pain reliever/anti-inflammatory. Most of us are also majorly Magnesium deficient. There are bio-identical creams on Amazon that are Vitamin D/Magnesium/Vitamin K and they really help for many things. Anyways, I sure hope I helped you out with some of my advice. I hope yours goes away soon! Mine is associated with my Fibromyalgia, so unfortunately, I think I’m just stuck with it indefinitely . Good luck!
NORMA SAUNDERS
Posted at 22:56h, 21 AprilI HAVE PAIN AT THE TOP OF THE LEG, HURTS TO WALK. ALSO BUTTOCK PAIN.
Dr. Chris
Posted at 23:03h, 21 AprilHi Norma, where at the top of the leg? How long have you had it? Is it achey, burning, stabbing, sharp, numb, tingly? How bad on a scale from 0-10?
Wendy Jackson
Posted at 00:11h, 10 MayHi
I had Lung cancer in 2010 with removal of left lung then in 2012 I had total hip replacement with Femoral nerve damage…at this time i can touch/scratch above knee… I have pain and heat..(in left outside of hip..sore to press..also pain in groin area, walking is hard anyway as I limp … this pain has been with me approx 4-5 years…I cant sit on the floor… or do lunges etc…and Doctors look at you like your a hypochondriac…. I know pain…and can live with a lot..as i have any help would be great
Thanks Wendy
Dr. Chris
Posted at 13:01h, 10 MayHi Wendy, you are absolutely not a hypochondriac. This pain is very real. The “heat” is not necessarily joint or muscle related. It could be the femoral nerve, although this would be the front or inside of the thigh (not the outside of the hip). Have you looked into finding someone to remove adhesion from your hip? With a total hip replacement, you definitely have a lot of it. With gratitude, Chris
Leslie Weller
Posted at 12:39h, 23 MayI find that my trochanteric bursitis comes and goes and seems to vary with my consumption of vitamins K2 and D supplements. I’m not certain yet, but I think the K2 is helping reduce calcification in the bursas. My issue is in both hips always at the same time.
Dr. Chris
Posted at 12:45h, 23 MayHi Leslie, I’m glad that helps you. Supplements like that will merely change the PAIN THRESHOLD of your problem, not address the issue itself. Because if it were truly a vitamin deficiency, you’d have pain in every joint (not just your hips). Keep dialing in your D + K2, but if you want healthy hips 30 years from now, remember to address the mechanical components of your hip too.
Sherry
Posted at 14:54h, 29 JuneHi Chris. I hired a not yet certified personal trainer about 6 years ago. I had been an extreme couch potato for about 15 years. He had me start with pretty advanced cardio and strength (as I later learned). I injured myself doing “throw-downs” with him. I felt 2 pops, inner thigh at crease of leg. At the time, I believed it was a groin pull. But from the moment of injury until now, pain upon standing or slowly walking that travels halfway down my thigh, stops there and continues to build in intensity until complete numbness occurs from hip to toes in that right leg. Had a hip mri done a few weeks ago, which does show bursitis. I’m worried about long term nerve injury and function. Doctors are telling me physical therapy but after 8 weeks hasn’t helped and might actually seem worse. My question- will foam rolling help? And any other suggestions would be much appreciated.
Sherry
Dr. Chris
Posted at 15:17h, 29 JuneHi Sherry, I’m sorry about your pain.
Here is what you said that makes me fairly confident there is a labrum and cartilage issue in the hip beyond “Just bursitis”:
– “pops”
– Pain that the inner thigh, especially with simple standing or walking (which isn’t putting stress on your groin)
– “numbness” – this is a NERVE symptom, not a “groin pull” [I don’t know the exact location when you describe hips to toes, so it’s hard for me to tell which nerve. My best bet right now is that it’s coming from the low back)
I would not recommend more physical therapy. Doctors prescribe this because they don’t know what else to do.
Where do you live?
It’s time to find a specialist. You can look for a provider on integrativediagnosis.com. There aren’t many of us, but no one trains like ID providers.
Alexandra Higgins
Posted at 14:02h, 24 JulyHi
I have bursitis in both my hips which csn sometimes radiate from the side of my thighs and the front of my lower leg to my foot. Very painful after and during walking uphill, can’t lie on them at night and also a stiff lower back.
I walk a lot, do yoga and have an active job but the pain is really impacting this. I have been suffering for 10years I am not overweight, eat healthuly I have been to ostiopath,chiropractor, had acupunter,pulsed light and physio. Nothing has worked.
Can’t seem to get to the bottom of it.
Any suggestions?
Alex x
Dr. Chris
Posted at 23:56h, 30 JulyHi Alexandra, I’m sorry for your struggle.
How was the bursitis diagnosed? “Bursitis” doesn’t refer to the leg/foot. That radiation is something else.
Yeah, you don’t have the capacity to do all that movement.
Have you measured the 3 tests above?
Jessica Harvey
Posted at 14:41h, 13 MarchI had an MRI that showed I have Baastrups Disease and feel I am dealing with bursitis now down my leg. I wondered about graston method to help with the leg issue? Is heat or ice best? I walk a treadmill 40 minutes a day 6 days a week. I also just had my 60th birthday. The oldest Jessica you will meet 🙂
Dr. Chris
Posted at 11:03h, 12 AprilNo graston. You’ll need hands on treatment for legs. Graston won’t get deep enough. Heat best for chronic issues. : ) Keep walking!
Jeff Klassen
Posted at 20:22h, 13 AprilHi Chris,
I am a 25 year old male. I am a land surveyor by trade and do a lot of walking. My doctor diagnosed me with bursitis based only on my description of the injury. The pain is at the bottom of the hip bone on the right side. He has me on Naproxen but told me stay away from physical therapy as it could make it worse. I appreciate your article. Makes sense to get behind the cause of the original pain. Thank you
Dr. Chris
Posted at 23:39h, 13 AprilYou’re very welcome Jeff. Yeah, that’s ridiculous. I’d stop the naproxen and see a doctor who knows what they’re doing.
Jeanette Jackson
Posted at 19:38h, 08 SeptemberI suspect I might have bursitis in my right hip.
I first noticed calf pain/tightness earlier this year and suspected a DVT as the discomfort seemed to appear after a long haul flight. However scans did not show any blockage or evidence to support this etc. Therefore I presumed I had pulled a muscle when rushing across the airport to catch my flight.
This was then replaced about three months later by a dull, persistent and gnawing throbbing type ache in the back centre of my thigh of the same leg (The area being about the size of an orange). After about a month of this discomfort I then noticed a dull pain in my lower outer buttock and hip which often was worse after sleeping on that side.
Also I noticed that when I put weight on the hip/buttock by sitting on the edge of a chair, the area of discomfort and pain became heightened with a sharper pain and the pain/discomfort appeared to radiate from inside my hip joint. The discomfort is usually worse in an evening, however it is pretty much constant and I’m also still getting the throbbing discomfort in the back of my thigh.
I have not been to the doctor or taking any medication for this and am just trying to elevate my leg as much as possible.
What are your thoughts?
Dr. Chris
Posted at 10:35h, 09 SeptemberSounds like a highly probable disc injury. If the calf symptom was numb, tingly, or lightning, the nerve root is involved. If not, then it’s a disc with “sclerotogenous referral.” I’d get the adhesion removed around your discs and the symptoms will go away.
Ern
Posted at 00:12h, 17 AugustDo you take medicaid? Thank you
Dr. Chris
Posted at 19:07h, 17 AugustI’m sorry we don’t. Medicaid is government insurance and only pays for chiropractic adjustments which we do not do.
Nellie
Posted at 00:42h, 17 AugustHi Dr. Chris:
64 y.o female. Hip pain for about five years, finally diagnosed with torn labrum and bursitis. I was told “we only operate on younger people, you would not be happy with the surgery, it does not cause that much pain anyway.” “okay” I thought, you’re the docs, the experts, now what about the bursitis?” Several shots, nothing worked, physical therapy three separate times, faithfully show up to every appointment. In all honesty, I thought pt was a joke. I get more exercise taking out the trash. I have been an avid swimmer all my life, like to use my tread mill and they just had me shuffle around in a heated pool. But I did what they said. I am looking at your exercise recommendations and starting to do them. What is your take on all this torn labrum stuff?
Dr. Chris
Posted at 19:08h, 17 AugustHi Nellie,
So sorry about the care you received. We treat torn labrums all the time. Bonnie is younger, but you can see the results that are possible.
https://youtu.be/r49ewo4SN4w