01 Feb The Truth About Achilles Tendinitis (And Achilles Pain)
Does your Achilles tendon hurt? You probably don’t have achilles tendinitis.
If I were a gambling man, I’d bet you have achilles tendinosis.
**Note: 97% of achilles tendon tears had a non-symptomatic achilles tendinosis present. If you want to minimize the risk of this severe rupture, read on.
Why It’s Not “Achilles Tendinitis”
I already wrote about the difference between fasciitis and fasciosis in the plantar fasciitis post.
Here, I will write similarly about tendinitis and tendinosis.
The “-itis” ending in tendonitis or fasciitis implies “inflammation.”
Inflammation is the natural bodily process of attempting to heal. It is normal and healthy in musculoskeletal conditions such as a bruise on the arm or a torn hamstring.
It isn’t normal when the body is in a hyper-inflammatory (“hyper”= too much), usually through a diet consisting of grains (that include gluten), processed dairy, and lots of sugar.
The hallmark signs of inflammation are:
- rubor – redness
- tumor – swelling
- calor – heat
- dolor – pain
In most tendon issues, the only hallmark sign of inflammation that is present is pain. None of the others show.
Due to this finding and contrary to popular belief, most tendon or fascia issues are not “-itis”or inflammatory issues but “-osis” or degeneration issues.
In general, what does degeneration or tendinosis look like?
When prosectors open up the fascia in anatomical studies or biopsies, inflammatory cells are not found, confirming that there is no “-itis”.
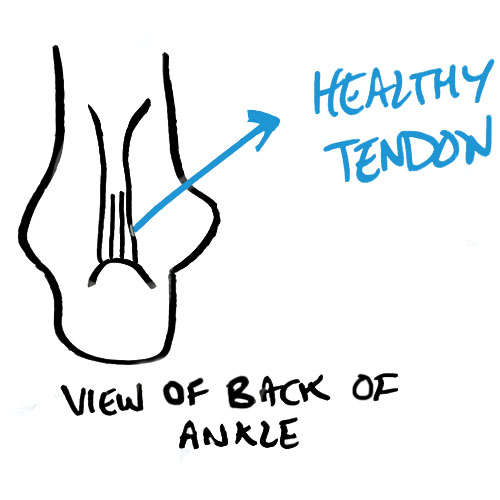
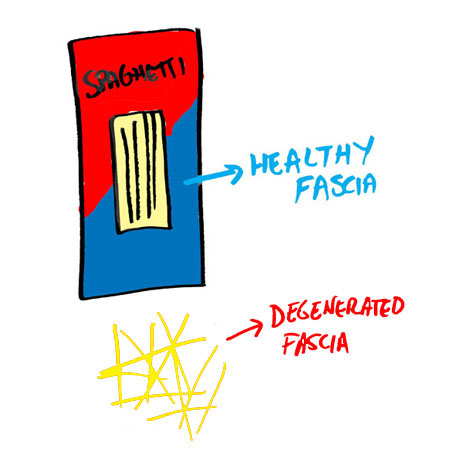
Observe the window of a box of spaghetti. Notice all of the spaghetti are lined parallel to eachother, straight up and down. This is what a healthy tendon looks like and how the fibers are oriented in a normal, healthy tendon. One that can handle the load you put on it when you’re walking, running, sprinting, or jumping.
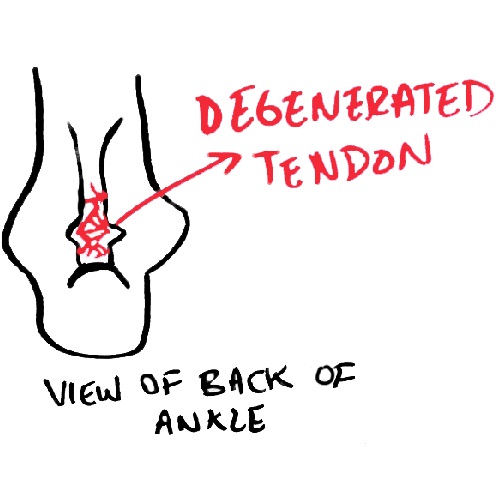
Now take the box of spaghetti and cook it or worse, throw it on the ground (and waste it). After either event, the spaghetti will no longer be parallel, but going in every which way direction. This is what a degenerated tendon looks like and how the fibers are oriented in a sick, diseased tendon. One that can not handle the load you put on it (and lets you know with the fire alarm that is “pain”) when you’re walking, running, sprinting, or jumping, leaving you at risk for further degeneration or worse, a tear or rupture.
How to Diagnose Tendinosis
Achilles tendinosis occurs when a tendon is either overloaded (too much work) or underloaded (not enough work) over time. Acute inflammation would occur implying tendinitis would be a result of overload over a much shorter period of time.
Achilles tendinosis can develop in a runner who does fifty miles a day or in a tv-watcher who watches fifty tv shows a day.
Achilles Tendonosis is usually diagnosed under 4 conditions:
- Location – Achilles tendon, most often just above the attachment point at the calcaneus.
- Palpation – The achilles tendon, 1″ above the insertion into the calcaneus, will thicken when degenerated. This is a **key** finding differentiating the two diagnosis and is something any qualified diagnositician will pick up.
- Range of Motion – Normal ankle dorsiflexion range (test your own ankle dorsiflexion range of motion here) of motion is 5-7″. Someone with achilles tendinosis will usually present with a much decreased range due to adhesion in the deep calf structures listed below.
- Symptoms specific to the timing of load – Nirschl Tendinosis Pain Phases.
Nirschl’s Pain Phases are symptoms letting you know how far your tendon has broken down. The cool part of this is as symptoms progress and an individual wants to simply continue working (and putting load on their body), then we can say objectively “Your body is breaking down. You’re on a path towards greater damage. How far do you want to take this?”
- Phase 1: Mild pain after exercise, resolves within 24 hours.
- Phase 2: Pain after exercise, exceeds 48 hours, resolves with warm-up.
- Phase 3: Pain with exercise that does not alter activity.
- Phase 4: Pain with exercise that does alter activity.
- Phase 5: Pain caused by heavy activities of daily living.
- Phase 6: Intermittent pain at rest that does not disturb sleep, and pain caused by light activities of daily living.
- Phase 7: Contsant rest pain and pain that disturbs sleep.
Pain phases 5, 6, and 7 indicate increasing percentages of permanent tendon damage.
Looking at these pain phases, you should be able to determine where you are on the pain scale. Once you get to Phase 4 or later, you will not be able to determine between tendinitis and tendinosis according to symptoms provocation as both cases will have symptoms increased with any activity. If you’re currently suffering from achilles pain, you may have to think back into the past to remember if Phases 1-3 of tendinosis were present to determine if tendinosis is the diagnosis on your own.
Conventional Management of Achilles Tendinitis
If the diagnosis were “Achilles tendinitis”, Wikipedia’s list of treatments would include:
- ice
- cold
- compression therapy
- wearing heel pads to reduce the strain on the tendon
- eccentric Achilles tendon strengthening
- NSAIDs
- ultrasound therapy
- manual therapy techniques
- rehabilitation exercises
- plaster cast application
- steroid injection
- autologous blood injections
- prolotherapy
- extracorporeal shockwave therapy
The four conditions listed above are enough to diagnose Achilles tendonosis. The issue with this list of treatments is that it does not address the correct diagnosis, only providing a plethora of random solutions.
Let’s look at the list again.
- ice – implies “inflammation” is a problem and that the body doesn’t know what it’s doing in bringing immune system cells to the area of damage.
- cold – implies “inflammation” is a problem. But we’ve already clarified how achilles tendon-ITIS is not caused by inflammation, because the correct diagnosis is achilles tendon-OSIS caused by degeneration.
- compression therapy – implies “a lack in pressure”. Compression through the form of sleeves can help reduce symptoms by improving the elastic ability of muscles to stretch or contract. Again, this is not addressing the cause of the problem though.
- wearing heel pads to reduce the strain on the tendon – implies that “tightness” is a problem, which is often very true with ankle dorsiflexion. While this treatment tool can reduce symptoms, it’s not getting rid of any pathology.
- eccentric Achilles tendon strengthening – implies “weakness” of the tendon is an issue. Actually, eccentric exercises greatly increase the effectiveness of treatment. I like to recommend 2 sets of 15 reps of this exercise. A 1-3 on the 10 point pain scale (with 10 being the worst possible pain) is ok and helpful in this case. When no symptoms are experienced, you can increase the load with a backpack full of weights.
- NSAIDs – implies “inflammation”. These medications are not worth it. Google “NSAIDS and gut health” and you’ll see why.
- ultrasound therapy – I learned all about ultrasound in chiropractic school. I don’t even bother with it.
- manual therapy techniques – implies that “soft tissue” is a problem. Now, we’re getting somewhere. Do be weary of regular massage. Stick to ART for the calf and ART/Graston for the achilles tendon and plantar foot.
- rehabilitation exercises – implies that “weakness” is a problem. Weakness can be involved, but not often.
- plaster cast application
- steroid injection – Skip it! Studies show that they result in decreased tendon strength and only make the tendon worse!
- autologous blood injections – A procedure where they inject your blood into the symptomatic area. Results are variable as this is a fairly new procedure.
- prolotherapy – Another fairly new procedure that appears to have some positive results.
- extracorporeal shockwave therapy – A last new procedure that may prove effective as well.
How To Successfully Treat Achilles Tendinosis (Almost) Every Time
If the interventions for plantar fasciitis were working, patients wouldn’t go from podiatrist to podiatrist, year after year, looking for answers our patients do. The key to fix tendinosis (Wikipedia) is to currently identify each individual dysfunction and provide a sweet-spot solution for that dysfunction, not to shotgun a complaint with everything and see what works.
The NUMBER 1 problem in achilles tendonosis is that the tendon has started to degenerate and its fibers orient in a haphazard fashion due to scar tissue in the plantar fascia and deep calf stabilizing muscles.
Legitimate secondary problems are non-optimal bone alignment, scar tissue in the calf structures (tibialis posterior, flexor hallucis longus, flexor digitorum longus, flexor hallucis brevis), and risky activities of daily living.
Knowing what all of these problems are, a sweet spot solution needs to be delivered for each problem.
- The NUMBER 1 solution for achilles tendonosis: Active Release Techniqueor Manual Adhesion Release – the best technique to remove scar tissue from the body. The achilles tendon is a location where instruments such as Graston work very well, but the tools can only be used on superficial tissue (within one inch of the skin). Graston would not work well on the deep calf structures mentioned above.
- Load Management (Orthotics) – to correct bone aligment between the second metatarsal and the tibia. As much as I used to believe that everyone should be walking around barefoot, faulty bone structure proves this belief wrong. I learned this the hard way through destroying my own ankle with barefoot running. I use Sole Supports in practice.
- Load Management (Modification of Activities of Daily Living) –the body needs to be loaded just the right amount to be healthy. Overload (running too much without sufficient time for recovery) or underload (sitting for eight hours a day) won’t keep the spaghetti lined up nicely in the box. Only in introducing movements such as squats and lunges into an exercise program, taking breaks from sitting, managing the amount of running one days we can prevent this problem from developing in the future.
- Increase Capacity (eccentric Achilles tendon strengthening) – Tendonosis is one condition that responds very well to eccentric exercises. I like to recommend 2 sets of 15 reps of this exercise. A 1-3 on the 10 point pain scale (with 10 being the worst possible pain) is ok and helpful in this case. When no symptoms are experienced, you can increase the load with a backpack full of weights.
Here’s the big picture: if you think you have achilles tendinitis, actually have achilles tendonosis, and you’re not getting the scar tissue addressed through manual therapy, you’re not addressing the main problem. Your symptoms may go away with Wikipedia’s interventions, but I’m confident in saying they will return.
You can find providers near you by clicking on the appropriate link: Active Release Technique, Graston Technique, and Sole Supports.
 How long have you had your Achilles symptoms? What have you tried and has it worked?
How long have you had your Achilles symptoms? What have you tried and has it worked?



The Truth About Achilles Tendinitis (And Achilles Pain) | Primal Docs
Posted at 15:19h, 01 February[…] The Truth About Achilles Tendinitis (And Achilles Pain) […]
Foot Positioning in the Squat and Ankle Dorsiflexion Range of Motion
Posted at 21:26h, 15 June[…] your own terms. Especially if you’ve already overused your leg tissue enough to develop an achilles or plantar fascia […]
Amber Dean
Posted at 23:44h, 21 SeptemberCould we talk more about my Achilles pain via email? I’ve got some follow up questions after reading your article!
Dr. Chris
Posted at 19:34h, 22 SeptemberYes. : ) Check your email.
El Harper
Posted at 06:39h, 03 FebruaryIs the eccentric exercise you recommend contra-indicated with a dorsal bone spur? If so, what is an alternative?
Dr. Chris
Posted at 19:08h, 03 FebruaryNot contra-indicated, but if the pain is more than a 1 out of 10, your tendon OR spur can’t handle it, then you can try doing this eccentrically while sitting with a band under the ball of your toe.
Ian B
Posted at 23:00h, 15 JuneFantastic article. About 5 years ago I blew up either my Achilles or calf muscle trying to make a cut to catch a frisbee in shin high water and I have not been right ever since. Lately if I even walk for longer than 10 minutes it begins to hurt. Have seen two Orthopaedic surgeons and both say surgery is not the answer. Went to a physical therapist with no success. Really intrigued by ART but my concern is perhaps I am in phase 5-7 you outlined above and I am doomed to deal with this forever. Thanks again for the insights.
Dr. Chris
Posted at 10:07h, 16 JuneYou’re welcome. What does the MRI say exactly?
Eveen if it is Phase 5-7, Manual Adhesion Release is your best bet to fix this. I’m obviously biased, but take that for what you want.