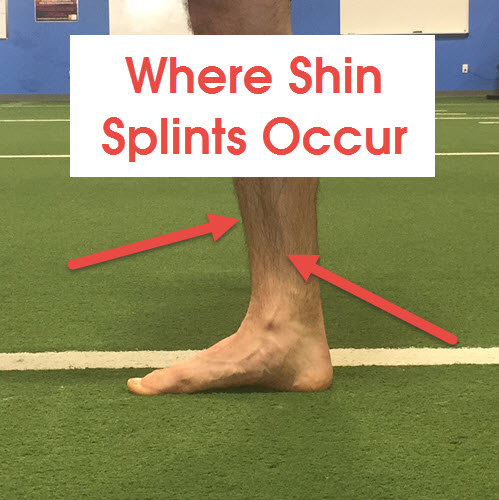
15 Nov A Guaranteed Guide to Fixing Shin Splints
Shin splints can be like playing tag with your friends when all your little brother wants to do is tag along: growing in annoyance the longer he’s around.
Shin splint sufferers are often given traditional advice that includes electronic stimulation, ice, heat, ultrasound, extracorporeal shockwave therapy (ESWT) and strengthening.
If that were working really well, there’d be no need for this overwhelming guide to shin splints.
By reading this, you’re setting yourself up to be out of shin splint pain in the near future. Guaranteed.
My intention here is not to overwhelm, but to give you as much knowledge you need to get rid of your shin splints, once and for all. Feel free to skip around sections to address what you “need to know.”
If you want to stop reading now and desire maximum value from this post, do this one thing: measure your dorsiflexion. Restriction with this range of motion is most correlated with pain below the knee.
What are Shin Splints?
“Shin splints” is a catch-all condition for pain between the knees and ankles.
They tend to occur on the front or inside of the shin bone.

It is an overuse condition, often caused by excessive running. Before we go any further, a couple of definitions:
- tissue: a group of specialized cells i.e. muscle, bone, fascia, ligament and tendons.
- dysfunction: musculoskeletal term for a “problem” i.e. strain, tear, adhesion, fracture
The list of tissue-specific dysfunctions that can be going on with your shin splints includes:
- muscle strain
- muscle tear
- fascial adhesion
- bone stress fracture
Note: If you want to know which muscles tend to be in pain, the front of shin muscles are tibialis anterior or the extensor group. On the inside of the shin, it’s flexor digitorum longus.
In the milder stages, you probably have less intense pain that began days to weeks ago. Short-term pain can be caused by a muscle strain or fascial adhesion.
In the later stages, you probably have more intense pain and it began months to years ago. Long-term pain can be caused by a muscle tear or a stress fracture.
Are you thinking “Enough with the rants Chris. I want to fix this now!” Skip down to the Level 3 Actions below. While a precise diagnosis may not be necessary to fix your shin splints, it is the fastest and most permanent way to be out of pain.
Down The Shin Splint Rabbit Hole
Determining the specific cause of shin splints is easier than determining which dysfunction you have. This part is vital if you’re going to attempt to fix your shin splints yourself. Without that knowledge, you’re hitting your hammer at screws and nuts and wondering why you’re not fixing your shin splints.
Let’s discuss the causes.
Shin splints are caused by:
- Tightness
- Weakness
In regards to tightness, two joints take priority in shin splints. The order is important:
- Ankles
- Hips
If you don’t have a minimum of 5″ of ankle dorsiflexion range of motion (you can figure this out in 60 seconds with the Knee to Wall Test), you’re ankle is too tight.
Measuring this range of motion is the most important thing you can do to determine the health of your calf, shin, and ankle.

Two more definitions for you:
- capacity: how much work your body can do. Picture a bucket. That’s your capacity.
- load: work your body does. Imagine putting water in your bucket. That’s you loading your body.
You need 5″ of ankle dorsiflexion because when you walk, your knee needs room to move over the front of your toes as your other leg swings though (just like in the picture above). When you run, you need even more room because running uses the greater spectrum of your range of motion than walking. If you don’t have that room, your calf and shin muscles will contract excessively (and lead to overuse) to avoid the range of motion you don’t have. Unnecessary contraction puts more water in your bucket than is ideal, causing you to spill out of your bucket more easily (and you feel symptoms such as pain or tightness) than a person without shin splints, who has a big enough bucket to hold all of the water.
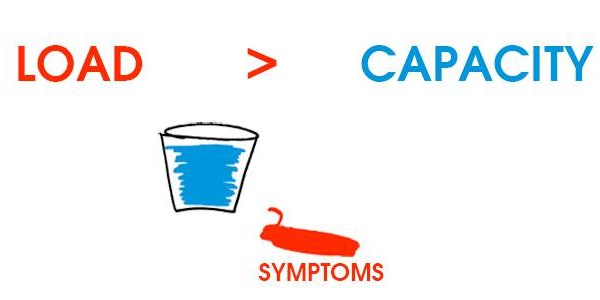
That’s just the ankle.
Let’s move up to the hip.
If your thigh cannot touch your ribs (you can figure this out in 60 seconds with the Thigh to Ribs Test), you’re hip is too tight. This tests hip flexion.

If your hip cannot come forward 12″ over your knee (you can figure this out in 60 seconds with the Lunge Stretch Test), you’re hip is too tight. This tests hip extension.

If you don’t have full range of motion in either direction, what do you think happens to the muscles around the hip and ankle?
Imagine you’re watching a runner run.
Notice how when her knee swings through, her thigh comes towards her ribs (replicating the Thigh to Ribs Test). Imagine that she is restricted and her thigh cannot come towards her ribs. She’ll take shorter strides as a compensation. The problem with the compensation is that she isn’t fully using the propulsive motor of the strongest joint in her body, the hip. With a smaller range of motion, her butt and hips cannot fire to move her forward. If you haven’t guessed what compensates for the lack of glute/ham firing, it’s her shin muscles.
Now, notice how when her leg swings backwards, her thigh moves behind her body (replicating the Lunge Stretch Test). If her thigh cannot move behind her, her strides will shorten even further. The shins will compensate even more and she’ll probably be putting excessive stress on her discs in her low back.
To prove my point, some of you weekend warriors reading this probably have low back pain along with your shin splints.
In a healthy, fit body, all of your muscles work at 100% of their abilities. Now, imagine you’re the runner. The three major joints that work in running are your hips, knees, and ankles. To run as long as possible as efficiently as possible, you need 100% capacity for all joints to work properly.
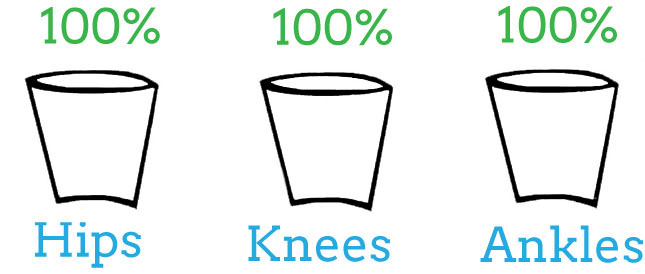
When you workout with a healthy body, all the joints are working together to keep the work (load) inside of the appropriate bucket.
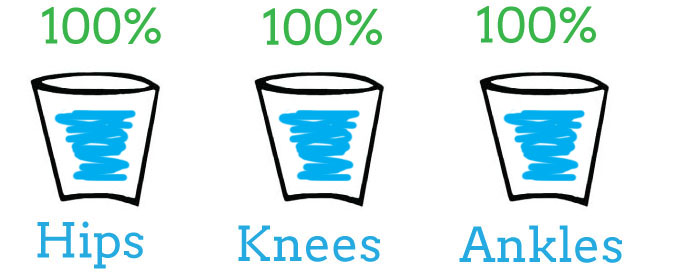
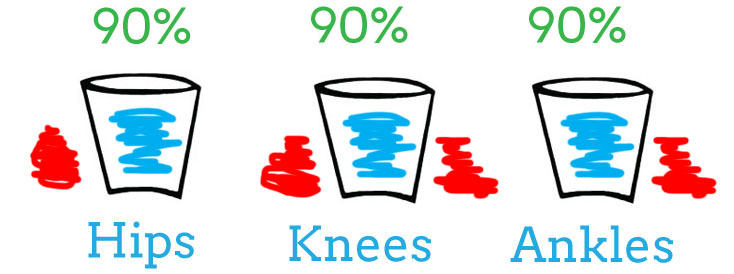
Now, let’s assume you injured your ankle (as evidenced by the red spilling out of the “Ankles” bucket in the image below).
Immediately, your body will take load out of the “Ankles” bucket and put it in another bucket. For simplicity again, I chose the “Hips”. In reality, the excess load can go to any number of joints or tissues. Notice, the ankles are now working at 90% capacity and the hips are working over-time at 110%.
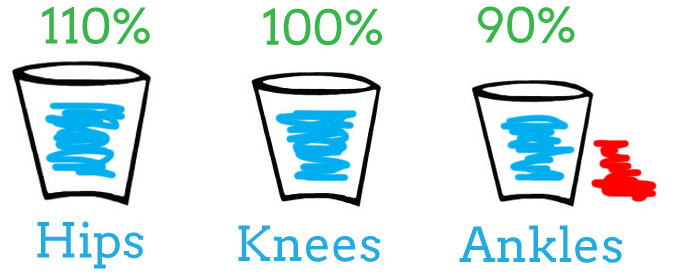
The body is amazing at compensating and will do so for as long as possible. Until that over-time joint gives up and now you have symptoms in two places, the hips and ankles.
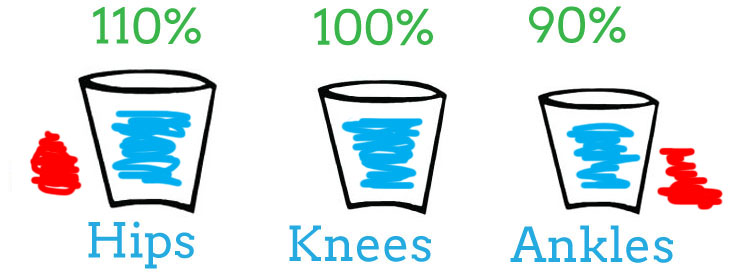
The hip symptoms indicate that now your “Hips” bucket is decreased in capacity. For simplicity, I chose 90%. Again, your body will compensate. As a runner, the only other place your body can put load is on the knees.
Notice below, instead of taking 10% more load, the knees have to take on 20% more load due to decreased capacity in both the ankles (10% decrease) and hips (10% decrease).
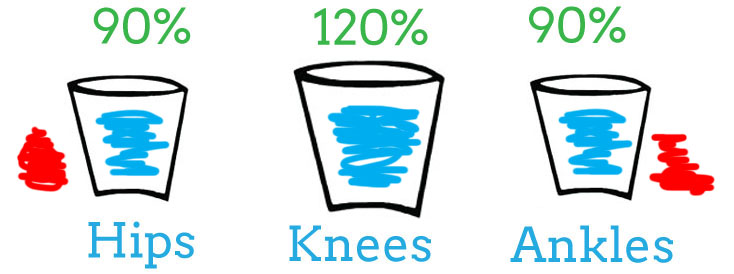
Your knees will compensate for as long as possible until they peter out too.
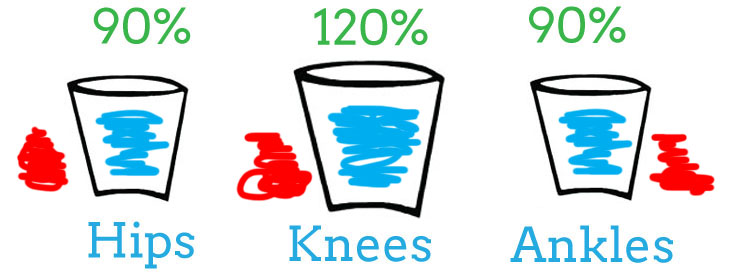
Finally, you notice your running times and distances are getting slower and smaller as there’s no where else to compensate, all of your joints and muscles are working at less than 100% capacity.
Thus, the Vicious Cycle of Muscle Compensation and Growing Pain continues.
The metaphor “When it rains, it pours” works here. Once one injury develops dysfunction in the tissue, the body has no choice but to use improper movement patterns to allow you to live, walk, stand, and move between sunrise and sunset. Your body will continue to exhaust your joints and tissues’ capacities until it has nothing left to use and you’re left saying:
I must be getting old, everything hurts.
The Vicious Cycle of Muscle Compensation and Growing Pain is the real reason why real treatment is so important. The Irrelevant Pain Relief Window has people thinking they’re healthy and fit after an intervention (stretching, foam rolling, strengthening, heat, stim, or any other thing that doesn’t address the dysfunction) to resume activity, only to be horribly let down.
If the story above resonates with you, this alternate paradigm of load, capacity, and respecting dysfunction will help you reverse the “aging” you’ve been experiencing.
What About Weakness?
With tightness out of the way, we can look at weakness.
Generally, if you cannot do 10 repetitions of a single leg heel drop slowly (video to come soon) at tempo, you’re too weak. This is the same sweet-spot exercise you would do if you had achilles tendinosis.
Now the question becomes why.
Weakness can be caused by a few things:
- Adhesion
- Protective Weakness
- Real Weakness
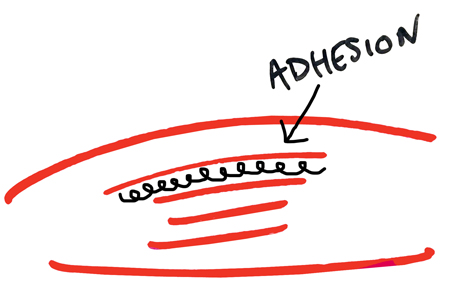
Adhesion: excessive connective tissue that acts like glue between your muscles.
Picture the steaks that are your muscles sliding and contracting as you walk or run. Now imagine that you took some gorilla glue and put it between the muscles of your leg. Can you see how your muscles wouldn’t want to slide, be flexible, or even contract?
Protective weakness: weakness caused by your nervous system shutting your muscles down to protect your body from further damage.
The most common place this occurs is with low back disc injuries.
Picture an individual picking up a pencil from the floor, only to drop his whole body on the ground. When the disc’s bucket is overloaded and the water spills out, the disc lets your brain know and your brain shuts you down so you don’t put more water in your bucket. That looks like all of this person’s muscles going weak as the person falls to the ground.
No one would say that this individual lost all of their muscle strength in a matter of seconds. The person who could deadlift 300 pounds and has this happen to them, does not lose their inherent muscle strength. They simply overloaded and damaged their disc to the point that the brain is over-riding whatever this person’s muscles are able to do to prevent further damage.
Real weakness: what people generally think of when you say “weak.” The muscle fibers themselves are not strong enough.
You know you have real weakness in your ankle structures when the following conditions are met:
- your Knee to Wall Test is 5″.
- experienced soft tissue provider finds no adhesion in your calves, shins, and feet.
- an x-ray and MRI come back clean, with no positive findings.
For each of these causes of weakness, a different solution is necessary. A hammer for a nail, a screwdriver for a screw, a wrench for a nut.
- Adhesion = removed by an experienced adhesion specialist, and then strengthened. (Doctor’s Note: Don’t bother trying to remove this yourself. It’s not possible. You need 6 pounds of tension per square inch to break adhesion. Tension is a parallel force to the muscles. Most tools use a compression force, which is straight down into muscles. None of the conventional tools out there create tension, besides an orthopedic surgeon’s saw and scalpel. I recommend you try an ID provider before going this route for obvious reasons. Surgery is invasive.)
- Protective Weakness = diagnosed to determine what tissue is damaged so badly that your brain is shutting you down, and that dysfunction must be treated.
- Weakness = strengthened.
You can’t hammer a screw. Your pain will continue.
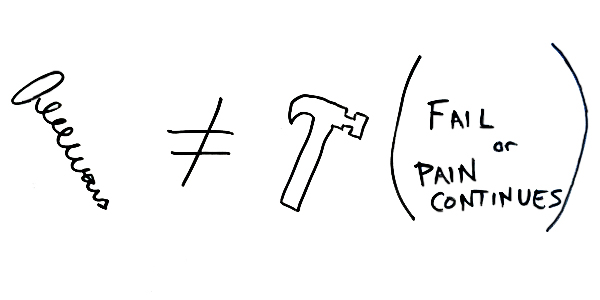
When you hammer nails, though, your pain goes away.
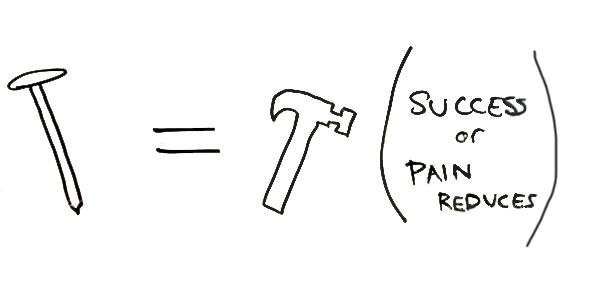
Let’s start hammering nails.
Do this: 3 Levels of Action
Depending on how intense your pain is and how long you’ve had your pain, I recommend 3 levels of action. The psychology of behavioral change warrants which action you’ll take based on the significance of pain in your life. At Barefoot Rehab, when we tell pain sufferers there’s no one better at getting rid of acute or chronic pain, they say “That’s nice” and they continue doing what they’re doing. We’ve stopped wasting our breath with acute injuries (lasting less than one month) that haven’t greatly affected someone’s life.
When that same pain sufferer has been to 3-5 other doctors and their pain is getting worse over months to years, then they’re ready to do whatever we say. This fact is the reason why we only market to patients who have been to 3-5 other doctors and they’re clearly annoyed and frustrated by the pain.
Back to you. If you operate outside of this normal world of “pain” because you’ve already cultivated the core values of health, longevity, and right action, then skip down to Level 3. It’ll save you time and energy. If you have your reasons for starting at Level 1, there is zero judgement. I hope it works and then we’ll all throw a happy party.
Level 1 Actions:
Level 1 is akin to you completely shooting in the dark, assuming you have “shin splints” based on one data point: the location of your pain. 80% of acute pain gets better, no matter which interventions you do. It makes sense why you would start here.
- Rest.
- Stretch.
- Strengthen.
- Get over-the-counter orthotics.
- Use modalities.
Common sense tells us that there is probably an inflammation component to your overuse. You can test this by resting your shins for a length of time. How much time is difficult to say. The longer, the better. If you resume activity after rest and notice you can do what you want to do for a longer period of time, then inflammation was a dysfunction on your pain graph and you effectively got rid of it.
Below is an example of a pain graph for someone with a bone spur. To fix pain 100%, every block needs to be respected. For now, just appreciate the complexity of pain here by observing all contributing blocks stacking on top of each other:
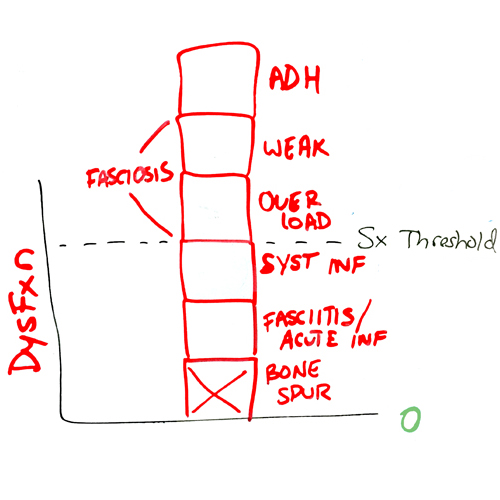
Stretching and strengthening are standard in the physical therapy route and are generally a good thing. Try both and see if your pain gets better. A simple youtube or google search of each will bring up specific exercises to do. Tactics aren’t important here. Just pick some.
If the pain is difficult to deal with, feel free to experiment with modalities. Ice, heat, ultrasound, electronic stimulation, lasers, shockwaves are all fair game when it comes to temporarily decrease your pain. Conventional physical therapists and chiropractors use these modalities. You can also get some modalities (like electronic stimulation TENS units) for at-home personal use.
One word of caution: Don’t use modalities, only to go run more, and create another vicious cycle of modalities and running. The cycle only goes down from here. Your dysfunction is growing in magnitude.
Did the Level 1 Actions work? Feel free to share in the comments below so others can benefit from your experience.
Level 2 Actions:
Level 2 presumes Level 1 did not work. The actions below allow you to start to collect more data points for your pain.
- Measure your ankle dorsiflexion with the Knee to Wall Test.
- Measure your ankle alignment by having someone observe your tibia-2nd toe line as mentioned in the Best Orthotics post.
- Measure your hip flexion with the Thigh to Ribs Test and extension with the Lunge Stretch Test.
- Measure your other lower body ranges of motion (Touch Your Toes Test, Face Up Heel to Butt Test, Face Down Heel to Butt Test).
- Work to increase your restricted ranges of motion.
When you know your numbers for joint ranges of motion, it’s like you’re assessing the blood pressure of your heart and blood vessels.
High blood pressure increases our risk of a heart attack. It’s common knowledge.
When our M.D. says to workout, eat better, or take a statin medication, we understand why and don’t object (unless it’s resisting the medication).
Most people don’t realize that measuring joint range of motion is like taking the blood pressure of that joint.
When you’re tight and restricted, you can make sense of your pain story to get out of pain now, permanently.
Do whatever mobility or stretching exercise you wish to attempt to restore your range of motion. It’s irrelevant which tactic you choose for this purpose.
Re-test in a month and see if your test has gotten better. If your range of motion has increased, great! Rinse and repeat!
If your test is the same, it’s time to go to Level 3 for more drastic.

Did the Level 2 Actions work? Feel free to share in the comments below so others can benefit from your experience.
Level 3 Actions:
If you’ve gotten here, either Levels 1 and 2 didn’t work or you want the highest level of care.
- Find an Integrative Diagnosis Provider.
- Get the best orthotics out there.
An Integrative Diagnosis Provider is skilled at two things that very difficult to come by:
- The complete, with no-stone-unturned, diagnosis of musculoskeletal conditions.
- Within that diagnosis, finding and removing fascial adhesion.
The amount of education these providers go under to fix people’s annoying and stubborn pain is second to none. I never saw this attention to detail in chiropractic school. In our practice, we’ve budget $20,000-30,000 per doctor for our own continuing education. Our colleagues around the world spend the same. There’s no one else who is so dedicated to getting their patients’ results when it comes to getting out of pain, no matter how long they’ve been suffering.
Go to the Integrative Diagnosis directory to find a provider near you. If there is no one near you and you really want to be out of pain, consider flying to one. It’s common for Integrative Diagnosis providers’ patients to fly in from other states or drive many hours in the car.
If you can’t find an ID provider near you, make sure you mention that you want these three deep calf muscles treated:
- tibialis posterior
- flexor digitorum longus (you may point to this spot if you have pain inside of the shin)
- flexor hallucis longus
I’m not mentioning the front of the shin muscles because if you point to that spot, I’m assuming the provider will treat that location.
As soon as the practitioner you’ve chosen to see says they’re treating soleus or the gastroc, run out the door! These tissues are rarely involved with shin splints or any other calf, shin, or foot problem.
Back to the guarantee. There are a few caveats to you fixing shin splints. If you have a massive structural ankle problem (as diagnosed by x-ray or MRI), continue to put water in your bucket (by refusing to stop activity while having adhesion removed), or fight the doctor with precisely what he tells you what to do, the pain will continue.
 What has your experience been with shin splints? Feel free to tell us below.
What has your experience been with shin splints? Feel free to tell us below.

No Comments