08 Oct I Don’t Care About Your Herniated Disc … or Do I? (How Perfect Are Lumbar MRI’s?)
Here’s what I had to say in 2015, when I was 5 years into practice.
I don’t care about your herniated disc. Or your torn labrum. Or the arthritis in your neck. ~Yours Truly
As I sit to edit this document in 2022 after practicing for 7 more years, I edit my above statement.
I care about your herniated disc in appropriate proportion as the other relevant puzzle pieces. Sometimes, I care a lot and sometimes I care a little. ~Yours Truly
Fixing your low back pain is what matters.
Chronic low back pain, by definition of being “chronic”, is hard to fix.
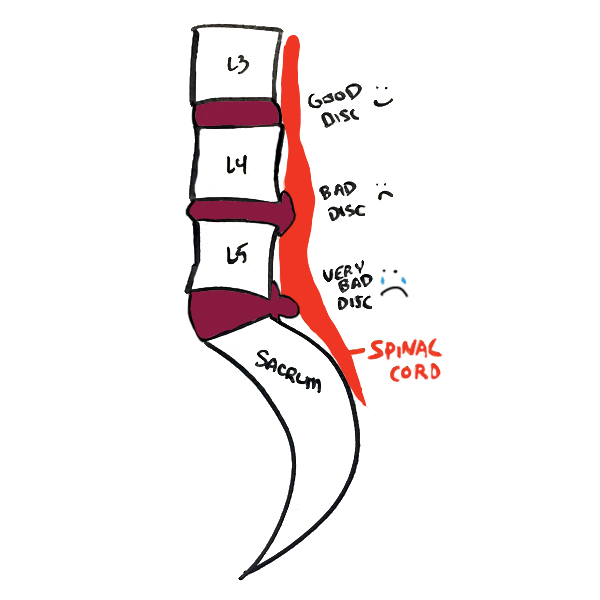
To have the best odds at fixing low back pain caused by herniated discs, it’s vital to have a complete diagnosis.
A horrible low back disc herniation as diagnosed by CT or MRI is not a death sentence just as a very clean image doesn’t mean you’re in the clear.
Our patient Natalie was scheduled for micro-discectomy for her horrible disc before deciding to get checked for adhesion first. Thank goodness she did because she was able to cancel her surgery!
Let’s discuss imaging as one piece of the diagnostic puzzle.
The Research on Herniated Discs
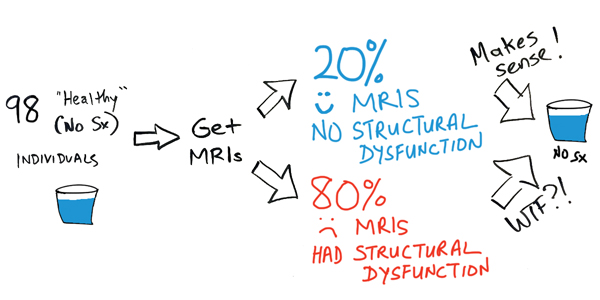
In a 1994 study by the New England Journal of Medicine, researchers sent images of 98 “healthy” (they had no symptoms) backs to two neuroradiologists, asking for a diagnosis.
Only 20% of the SYMPTOM-LESS individuals had clean MRIs. That means no herniations, sequestrations, extrusions, dragons, or monsters present.
52% had a bulge at least one level.
27% had an extrustion.
1% had an extrusion.
Conclusion: 80% of healthy people WITH NO SYMPTOMS had MRIs that a doctor diagnosed as a problem.
Second Conclusion: Approximately 85% of low back pain cases have no definitive diagnosis.
Let me summarize the research: There’s more to a complete diagnosis than just a healthy or unhealthy image.
What Does An MRI Do?
In a report done by the Radiology Society of North America in 2007, imaging has two roles.
- provide accurate morphological information (what the “structure” of the spine looks like and identify structural dysfunctions).
- influence therapeutic decision making.
No one denies that imaging such as MRIs successfully accomplish #1, at least a percentage of the time (more on this later).
The problem is with #2.
Any study looking at the natural history of degenerative disk disease, prognostic value of imaging, or its effect on therapeutic decision making will be confounded by the high prevalence of morphologic change in the asymptomatic population.”
[the boldness is mine.]
The MRI is relatively successful at taking a picture of the joints of the body.
Again, this is only one piece of the puzzle.
As a puzzle piece, we normally refer out for an MRI in these situations:
- at a consult or exam when an individual’s symptoms present with a severe disc pathology.
- when within 1-5 treatments have not produced permanent, sustainable relief in symptoms.
- serious trauma to the low back.
- lower extremity numbness/tingling that is not provoked by musculoskeletal movements.
- lower extremity numbness/tingling/weakness that is progressively getting worse.
- serious “saucerization” of the low back (more on this in another blog post. “Saucerization” is a fancy way of saying that the lumbar spine has been damaged and the muscles at specific levels won’t relax and stretch, either due to spasm or adhesion.)
In the above cases, an MRI can help let the doctor know if treatment should begin/continue or if surgery is the right solution.
This MUST be taken into context on an individual basis. Imaging such as MRIs are not perfect. But they can be helpful to determine what’s the best route to treat a patient.
Is MRI technology 100% Perfect?
Many people who get MRIs will tell us:
My MRI is clean – I’m so excited!
Well, hang on a second, Buster.
Let’s talk about sensitivity and specificity.
Sensitivity is how good is this technology at catching problems?
Specificity is how good is this technology at catching this specific problem – in this case, a herniated disc?
A 2012 review of 8 studies was done to determine the diagnostic accuracy of low back pathologies because 5% of all low back pain cases require diagnostic confirmation.
Researchers found a sensitivity level of 75% and specificity level of 77% for herniated discs, but results were inconclusive due to a small number of studies.
If this is correct, that means that 1 out of 4 disc problems will NOT be picked up by MRI and 1 out of 4 diagnosed herniated disc pain will actually be caused by another problem.
A 2018 review of 14 studies found similar results: 81% sensitivity and 77% specificity for MRI, CT, & myelography, although the quality of evidence was again, low.
As a practitioner, our conclusion here is that imaging is valuable, but isn’t the be-all, end-all. We must defer to symptomatic presentation in order to determine the best route of care.
Is Conventional Wisdom for Disc Herniations Correct?
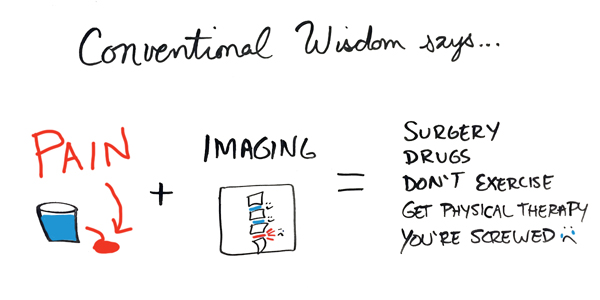
This equation is merely a moment in time and is missing depth and specificity to the puzzle.
At this moment in time, you’re in pain with a certain amount of structural change to your body (as evidenced by the MRI). The “answer” part to the equation is trying to protect you based on what conventional wisdom knows. Doing specific movements will only increase the amount of pain and damage done to the structure of your body.
Conventional Wisdom has served us human beings in the past by showing us that there were pieces of the puzzle that we didn’t know existed.
But CW is still missing diagnostic pieces.
What I Care About to Fix Low Back Pain
I often wonder at the above advice “How are you supposed to use the toilet bowl when the doctor says you’re not allowed to squat?”
That advice makes me realize, every healthcare practitioner is doing the best that they can.
The most holistic of practitioners are letting you know all of the pieces to your pain and health puzzle. He then let’s you know the best tools for putting those pieces of the puzzle together.
What I do I care about is completely and holistically identifying all dysfunctions, relevant pathologies, and pieces of your pain puzzle, which may include:
- other structural dysfunctions (ie. osteoarthritis, morphology issues of your hips like CAM or pincer malformations)
- the amount of adhesion (aka fuzz, bubble gum, scar tissue, or glue) in your soft tissue between your muscles, ligaments, nerves, and tendons as evidenced by flexibility tests like the:
- a lack of strength, endurance, and stamina of your muscles, especially in your Lunge.
- the level of system inflammation you have in your body from consuming inflammatory foods such as grains, dairy, sugar, processed foods, and artificial sweeteners (we recommend Chris Kresser’s paleo elimination diet).
- how much emotional stress you’re under, possibly leading to adrenal fatigue.
- how many hours of sleep you get.
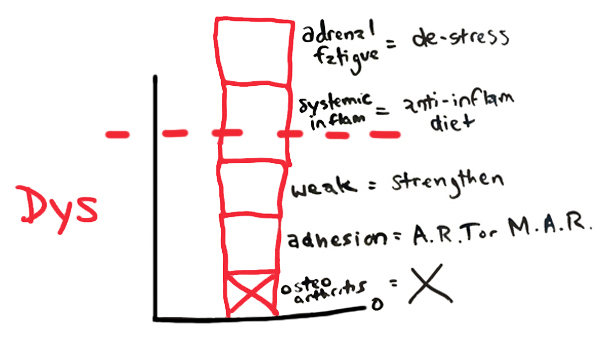
A graph of your dysfunctions and with sweet-spot solutions for those dysfunctions may look like this:
All of the diagnostic puzzle pieces (or blocks in the above graph) matter.
It’s the low back pain specialist’s duty to put these pieces together to determine the best route of care to help someone fix acute or chronic low back pain.
Take Home Message – Eat Your Humble Pie
Humble pie satiates you.
It tastes good when you digest the truth of your condition and state of life.
MRI’s aren’t throw-away data.
MRI’s aren’t data sitting atop a throne.
It’s an important diagnostic piece, but not the only diagnostic piece.

Spoonful by spoonful, here is what you can start to metabolize from above:
- An MRI is a helpful piece of information. But it means nothing without the other puzzle pieces.
- The most common cause of chronic pain in 30-60 year olds that no one is talking about is the dysfunction adhesion.
- Weakness, systemic inflammation, emotional health, and other medical conditions are other important puzzle pieces to consider.
There. A nice, healthy dose of perspective. : )
 We’re curious, what is your experience with the above? Please share comments below.
We’re curious, what is your experience with the above? Please share comments below.

Know Your Numbers: Standards for Musculoskeletal Health, The Low Back, And The Touch Your Toes Test
Posted at 15:54h, 14 December[…] already told you how I don’t care about the diagnosis of your “herniated disc” because it’s only one part (#4 below) of the diagnosis and pain […]
Case Study: Frozen Shoulder Success
Posted at 16:29h, 28 January[…] already written how I don’t care about your herniated disc and the truth about plantar […]
Stacy Dash
Posted at 14:33h, 30 MarchI have a herniated L4 and I’ve had 2 spinal injections. I have not gotten better. I want to be able to deadlift again. My doctor now says I have arthritis in my Facets.
What do I do, how do I heal and get back to the gym.
Dr. Chris
Posted at 14:59h, 30 MarchHi Stacy, I’m sorry for your pain.
Start with the pencil test and see how bad it is (https://www.barefootrehab.com/pencil-test-low-back-pain/).
If this is restricted, you’ll need to find an adhesion removal specialist.
If it’s not restricted …
How old are you?
How long have you been lifting?
Where is your pain?
Have you been resting?